Social Drivers of Health: A Framework for Improving Health Outcomes
Introduction
Hospitals and health care organizations are mission-driven to improve the health and well-being of the patients and the communities they serve. Because health is shaped by far more than clinical care alone, many hospitals are considering the impact of the social drivers of health on the communities they serve and the implications for care delivery. Social drivers of health are the non-medical factors that impact people’s ability to be and stay healthy. They include safe and stable housing, access to nutritious food, transportation, education, employment, social support, neighborhood safety, and clean air and water.
The scale and breadth of social drivers’ impact on health outcomes mean that hospitals and health care systems cannot address them alone. This reality is evident in daily clinical practice, where providers regularly see the impact of social factors on their patients’ health. These factors shape who walks through the door, how sick they are when they arrive and how well they do after being discharged. Patients experiencing unmet social needs often have higher emergency department utilization, more hospital admissions and readmissions, longer lengths of stay and more complex and chronic medical needs. Identifying and addressing social needs benefits patient care and serves as an avenue to meet hospitals’ strategic goals including improving quality and health outcomes, reducing avoidable costs, achieving goals of value-based care payment arrangements, and building community engagement and trust.
Social drivers of health also contribute to improving community health and economic status, chronic disease rates, people’s ability to engage in health-promoting behaviors, access to care and, ultimately, life expectancy. People who have safe housing, reliable transportation, stable income, healthy food, supportive relationships and safe neighborhoods are more likely to stay healthy, better manage chronic conditions and recover from illness.
Challenges related to social drivers of health are not the same for every community. Different regions and communities face different obstacles based on geography, local resources and economic conditions. Rural communities may face limited access to transportation, broadband and health services, while urban neighborhoods often grapple with housing instability, lack of access to nutritious food and concentrated poverty. Individuals with lower incomes encounter the greatest constraints across nearly all social drivers. Recognizing how these challenges vary across communities helps hospitals design their strategies to help the parts of their communities that need it most. By proactively aligning clinical integration with community level action around social drivers of health, hospitals can help foster conditions that enable their patients and communities to thrive.
The Unique Position of Hospitals to Address Social Drivers of Health
Hospitals and health systems are trusted and influential organizations that sit at the intersection of clinical care and community need. Attributes of hospitals that make them well-positioned to assist with social drivers of health include:
- Hospitals see the consequences of unmet social needs. Hospitals directly observe how housing instability, food insecurity, lack of transportation, unsafe environments and economic hardship present in their patients’ medical conditions. They also absorb the financial consequences in the form of more uncompensated care, worse health outcomes, and avoidable hospitalizations and readmissions.
- Hospitals have trusted relationships with people at vulnerable moments. Being ill or hospitalized is a vulnerable moment for many people. Care providers can connect with patients to build relationships that create the conditions for patients to share personal challenges in clinical settings that they may not tell anyone else.
- Hospitals implement data-driven interventions. Hospitals use data from clinical assessments and screenings to better understand their patients, while Community Health Needs Assessment data provide deep insight into the communities they serve. Together, these data can reveal population-level patterns and guide care and community-based strategies that integrate social drivers of health.
- Hospitals are anchor institutions. Hospitals use data from clinical assessments and screenings to better understand their patients, while Community Health Assessment data provide deep insight into the communities they serve. Together, these data can reveal population-level patterns and guide care and community-based strategies that integrate social drivers of health.
- Hospitals are adept at coordinating and partnering across sectors. Many hospitals already routinely collaborate with public health departments, social service agencies, behavioral health providers, payers and community-based organizations. This existing infrastructure makes hospitals natural conveners for multi-sector initiatives around social drivers of health.
Addressing social drivers of health in clinical and community settings helps create the conditions for healthier patients and communities, while bolstering the long-term financial sustainability of hospitals and health care organizations.
Social Drivers of Health: A Framework for Improving Health Outcomes
Many health care organizations are implementing strategies alongside community stakeholders to better understand and address social drivers and ultimately improve the health and well-being of their patients and community members.
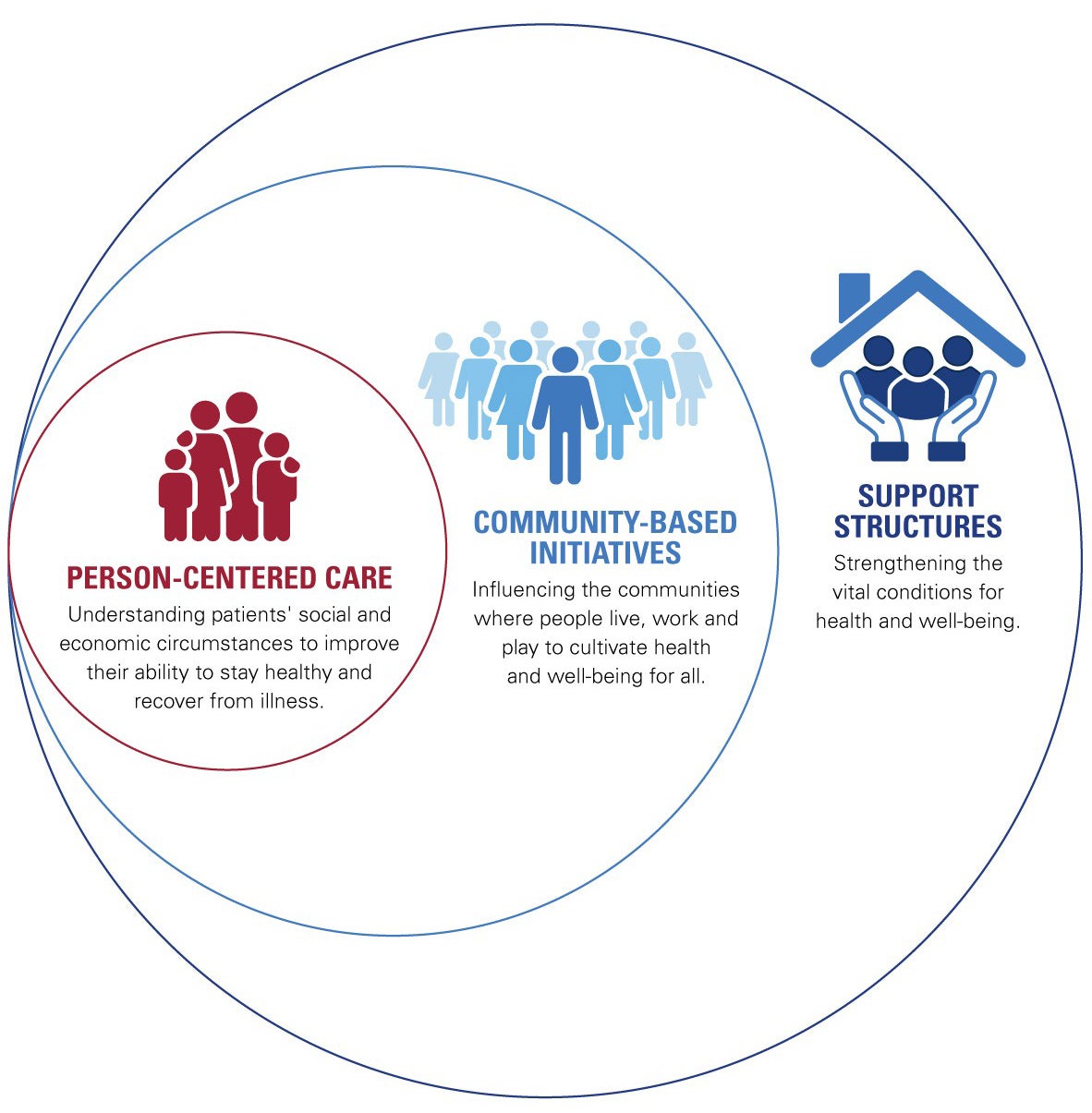
This Social Drivers of Health Framework presents a multitiered approach to inform hospital strategies by:
- Providing person-centered care in clinical settings.
- Participating in community-based initiatives, in partnership with multisector stakeholders, to influence the environment where people live.
- Bolstering support structures to foster the vital conditions for health and well-being.
Hospital and health care organizations can influence each level to drive better health for their individual patients and communities. Below is a description of each level and examples of what hospitals can do to advance the health of their patients and communities.
Person-centered Care
When providers understand patients’ social and economic situations, they are better able to support health and recovery from illness. Strategies hospitals may consider include:
- Screening for social and economic well-being to understand patients’ circumstances.
- Implementing referral systems to connect patients with additional support and resources as needed.
- Developing individualized care plans that integrate medical, social and economic factors in alignment with patients’ circumstances.
Community-based Initiatives
Influencing the communities where people live, work and play to cultivate health and well-being for all. Strategies hospitals may consider include:
- Conducting community health assessments and implementation strategies in alignment with other community stakeholders to identify priorities for action.
- Leading, convening, collaborating or supporting activities that create the conditions that bolster health.
- Strengthening community and multisector partnerships that build on local strengths and assets.
- Extending preventive and primary care into the community setting.
Support Structures
Strengthening the vital conditions for health and well-being. Strategies hospitals may consider include:
- Speaking to your local and state policy makers about how social drivers of health impact your patients and community.
- Investing in community infrastructure to create health-promoting conditions.
- Developing career pathways for the community-based workforce.
In Conclusion
As hospitals across the country consider how to address social drivers of health, they are developing individualized approaches to reflect their unique missions, capacities and community contexts. Given the complexity of these issues, progress is most effective when strategies are developed and implemented collaboratively with a range of stakeholders. This framework offers a perspective on how hospitals can incorporate strategies to address social drivers of health and contribute to meaningful, lasting improvements for the patients and communities they serve. It is intended to serve as a resource hospitals can adapt over time as community needs, partnerships and capabilities evolve.
More AHA Resources on the Social Drivers of Health
AHA Community Health Improvement