Fact Sheet: COVID-19 Related Payer Mix Changes Threaten 340B Hospital Eligibility
January 2022
The COVID-19 pandemic has altered hospitals’ payer mix, which for some hospitals has temporarily lowered their disproportionate share hospital (DSH) percentage. These changes have unfortunately threatened the ability of some hospitals to maintain their eligibility for the 340B program – a vital program that allows participating hospitals to stretch their resources to provide comprehensive services to their patients.
Background on the Issue:
The COVID-19 pandemic has ravaged the United States, with over 70 million people infected and nearly 900,000 people dead through January 2022. On the front lines of this devastating virus are our nation’s hospitals and health systems, which have collectively cared for over 4 million COVID-19 inpatients since the pandemic began. Mandatory shutdowns of non-emergent procedures to make way for increased demand for COVID-19 care resulted in strained financial and operational resources for hospitals across the U.S. These actions, while necessary, created an unfortunate consequence – significantly reduced patient volumes that altered some hospitals’ payer mixes, especially with respect to the proportion of a hospital’s patients that were insured through Medicaid or Medicare supplemental security income (SSI).
How Does this Impact 340B Eligibility?
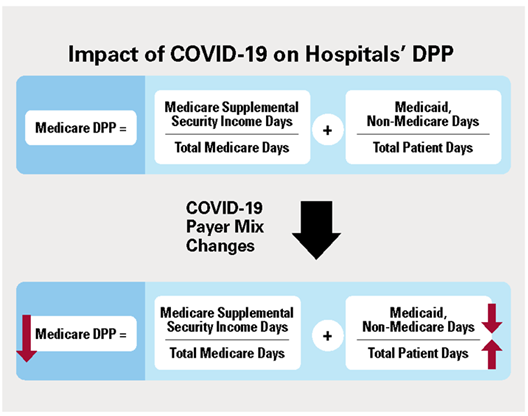 One of the primary eligibility criteria for hospitals in the 340B program is a measurement of the hospital’s volume of inpatient Medicaid and Medicare SSI patients, known as the “DSH Adjustment Percentage Threshold.”1 Hospitals report their share of patients who are Medicaid and Medicare SSI called the “DPP” on their Medicare cost report, which they file annually with the Centers for Medicare & Medicaid Services (CMS). A hospital’s Medicare DPP is then converted to a DSH adjustment percentage. The Health Resources and Services Administration (HRSA), which oversees the 340B program, uses the DSH adjustment percentage to determine 340B eligibility.
One of the primary eligibility criteria for hospitals in the 340B program is a measurement of the hospital’s volume of inpatient Medicaid and Medicare SSI patients, known as the “DSH Adjustment Percentage Threshold.”1 Hospitals report their share of patients who are Medicaid and Medicare SSI called the “DPP” on their Medicare cost report, which they file annually with the Centers for Medicare & Medicaid Services (CMS). A hospital’s Medicare DPP is then converted to a DSH adjustment percentage. The Health Resources and Services Administration (HRSA), which oversees the 340B program, uses the DSH adjustment percentage to determine 340B eligibility.
As patients have delayed care due to the pandemic, many hospitals are now seeing patients with higher acuity. A Kaufman Hall analysis indicates that this increase in patient acuity has driven an increase in patient length-of-stay at the hospital, up nearly 6% from pre-pandemic levels, which has also increased the total number of patient days (denominator; see graphic).2 At the same time, some hospitals are seeing a decrease in the number of Medicaid patients (numerator; see graphic) they are treating, resulting in a precipitous drop in their Medicaid ratio. For some hospitals this drop in the Medicaid ratio was not offset by any increase in the Medicare SSI ratio because CMS has not updated these ratios since the pandemic.3 As a result, for some hospitals the decrease in their Medicaid ratio has driven a decrease in their DPP and thereby has decreased their DSH adjustment percentage (see graphic).4
Why is This Issue Important?
 The 340B program was designed to help hospitals stretch their scarce federal resources to provide more comprehensive services to the patients they serve. Savings generated from the program are often used by hospitals to support important patient programs, such as diabetes assistance programs, medication therapy management and mental health treatment. Some hospitals, especially those in rural areas, use their savings to keep the doors of their facility open and to maintain important treatment services like infusion centers for cancer patients so that these patients do not have to travel far distances to access their treatments. As hospitals are forced out of the 340B program due to COVID-19- related changes to their DSH adjustment percentage, many of these important programs and services that depend on savings from the 340B program are at risk. The downstream effects of losing 340B eligibility will directly impact patients and their ability to access the care they need.
The 340B program was designed to help hospitals stretch their scarce federal resources to provide more comprehensive services to the patients they serve. Savings generated from the program are often used by hospitals to support important patient programs, such as diabetes assistance programs, medication therapy management and mental health treatment. Some hospitals, especially those in rural areas, use their savings to keep the doors of their facility open and to maintain important treatment services like infusion centers for cancer patients so that these patients do not have to travel far distances to access their treatments. As hospitals are forced out of the 340B program due to COVID-19- related changes to their DSH adjustment percentage, many of these important programs and services that depend on savings from the 340B program are at risk. The downstream effects of losing 340B eligibility will directly impact patients and their ability to access the care they need.
How do we Solve this Issue?
Congress or the Administration should act to ensure that 340B hospitals that were participating in the program at any point during the COVID-19 public health emergency and may have experienced changes to their DSH adjustment percentage due to the COVID-19 pandemic retain their 340B eligibility. Hospitals should not be penalized by losing their 340B eligibility due to temporary payer mix changes that were a direct result of the COVID-19 pandemic. Instead, programs like 340B that provide critical resources to hospitals should be safeguarded while hospitals continue to be on the front lines of the pandemic.
Legislation has been introduced in the Senate, S. 773, and the House, H.R. 3203, to provide 340B hospitals with certainty by allowing these hospitals to continue to access the 340B program during the public health emergency. In addition, the AHA continues to call on the Administration to provide this same flexibility through the 1135 waiver process. If swift action is not taken to address this issue, it is very likely that some 340B hospitals may lose access to the program, thereby jeopardizing care for the patients and communities they serve.
________________________
1. For hospitals that wish to participate in the 340B program as disproportionate share hospitals (DSH), free-standing children’s hospitals (PED), or
free-standing cancer hospitals (CAN), they must have a DSH adjustment percentage of at least 11.75%. For hospitals that wish to participate in the
program as either a Rural Referral Center (RRC) or a Sole Community Hospital (SCH), that threshold is 8%.
2. Kaufman Hall’s October 2021 National Hospital Flash Report shows a 5.5% increase in year-to-date length-of-stay compared to 2019 levels
(pre-pandemic).
3. CMS publishes Medicare SSI ratios that hospitals use as part of calculating their DPP and report these numbers on their annually filed cost report.
However, to our knowledge these data are lagged and CMS has not updated the Medicare SSI ratio such that it would account for any changes to
the ratio due to the COVID-19 pandemic.
4. Hospitals are required to notify HRSA, the agency that oversees the 340B program, if their DSH adjustment percentage falls below the required
threshold percentage. When this occur, the hospital must terminate from the 340B program.


