Addressing Societal Factors to Improve Health Equity

The COVID-19 pandemic has placed spotlight on health inequities in the United States. It has illuminated that, regardless of access to health care services, social and economic circumstances make some people more likely than others to become ill or have poor health. While this is not a new realization, and many hospitals and health systems have been addressing societal factors, the pandemic has created a true sense of urgency in understanding the role health care providers can play in improving health equity.
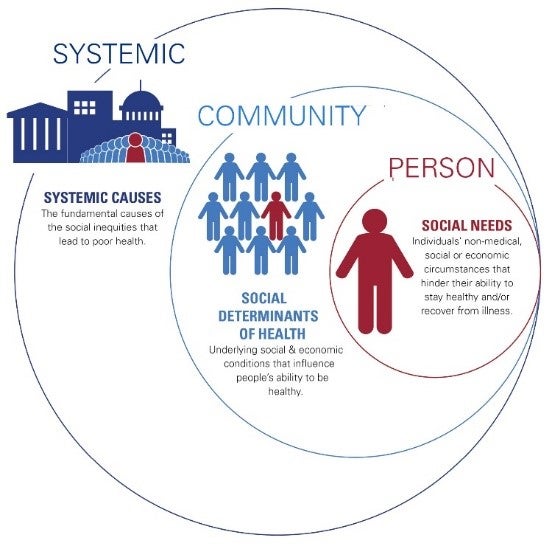 One pathway for improving health equity is to address the societal factors that influence health. AHA developed a new resource – Societal Factors that Influence Health: A Framework for Hospitals – to support hospitals and health systems as they take action to improve health equity. The framework sets forth three distinct, yet connected, levels that address patients’ social needs, social determinants of health in the community and the systemic causes of inequities. Each level offers actions hospitals can take to make progress towards health equity for their individual patients and communities.
One pathway for improving health equity is to address the societal factors that influence health. AHA developed a new resource – Societal Factors that Influence Health: A Framework for Hospitals – to support hospitals and health systems as they take action to improve health equity. The framework sets forth three distinct, yet connected, levels that address patients’ social needs, social determinants of health in the community and the systemic causes of inequities. Each level offers actions hospitals can take to make progress towards health equity for their individual patients and communities.
The framework’s first level is social needs – individuals’ non-medical social or economic circumstances that hinder their ability to stay healthy and/or recover from illness. Hospitals can screen patients for social needs and develop processes to connect patients with additional community-based or hospital resources. Screening for social needs can be paired with collecting race, ethnicity, language, sexual orientation and gender identity data that will allow hospitals to identify where health disparities exist in their population and develop strategies to address them.
The second level is social determinants of health – the underlying social and economic conditions in the community that influence people’s ability to be healthy. Because these issues reside at the community level, forming partnerships with other stakeholders in a hospital’s community will be crucial to addressing the social determinants of health. These partnerships can address a variety of social determinants, such as food deserts or a lack of affordable, safe housing options.
The broadest level of the framework involves systemic causes – the fundamental causes of the social inequities that lead to poor health. These include, for example, racism, sexism, generational poverty or redlining by financial institutions. At this level, hospitals can partner with other community stakeholders to affect policy, system, environmental or cultural changes that are connected to health at the local, state or national level.
As you develop strategies to address the societal factors in your community, you can look to hospital and health system leaders that have been on this journey for guidance. The AHA members we have talked to tie their progress to three fundamental principles:
- Hospitals cannot address all societal factors at one time – a step-by-step approach that is tailored to the needs of each community served works best. Start small and grow.
- Hospitals cannot – and should not – do this work alone. Finding partners in the community who can join this journey will lead to broader impact and success.
- Data is critical – it must be used to determine which societal factors to address and to measure the impact of the strategies to address them.
To further support hospitals and health systems in this effort, AHA offers a growing library of tools and resources to guide your journey at https://www.aha.org/societalfactors. And on March 16-18, 2021, you can virtually join peers from across the country for Accelerating Health Equity: A Virtual Conference for Leaders in Community Health, Diversity and Inclusion.
We are at a pivotal time for health equity in our country. Achieving health equity is a journey, and there is a path forward that will enable us to bridge the gap between commitment and action. As a health care field, it is our hope that we come together to address the societal factors that influence health so that all people can reach their highest potential for health.
Priya Bathija, J.D., MHSA, serves as AHA’s vice president of strategic initiatives. Julia Resnick, MPH, serves as senior program manager of strategic initiatives at the AHA.

