As Urged by the AHA, HHS to Allow Hospitals More Time to Spend COVID-19 Emergency Relief Funds
AHA Special Bulletin
June 11, 2021
HHS also made updates to other reporting requirements for PRF recipients
As urged by the AHA and other groups, the Department of Health and Human Services (HHS) today announced that it is extending the deadline by which hospitals and other providers that received Provider Relief Fund (PRF) money after June 30, 2020, must use their COVID-19 PRF payments.
The HHS announcement also extends the amount of time providers will have to report information on the use of their PRF money as part of other changes to PRF reporting requirements and clarifies which providers must report.
More details about the new deadlines and reporting requirements follow.
AHA Take:
In a statement shared with the media this afternoon, AHA President and CEO Rick Pollack said, “The Provider Relief Fund has been a life-line to hospitals, health systems and caregivers across the country, helping to keep our doors open during the pandemic in order to continue providing essential services to patients and communities. The AHA thanks HHS for listening to our concerns and extending the deadline for hospitals, health systems and other health care providers to use this critical relief funding. Today’s announcement to give some health care providers more time to spend emergency coronavirus funding will to help ensure that hospitals and health systems can continue the battle against COVID-19 as cases persist.”
Highlights of HHS’ Announcement on Provider Relief Funds
New Deadlines for Use of Funds
HHS has extended the deadline for use of funds (both for eligible expenses and lost revenue attributable to COVID-19) received after June 30, 2020. The deadline remains June 30, 2021 for any PRF funds received between April 10, 2020 and June 30, 2020. HHS notes that recipients may use payments for eligible expenses or lost revenue incurred prior to receipt of funds so long as they were used to prevent, prepare for, or respond to COVID-19.
The following chart provides the new deadlines based on four time periods.
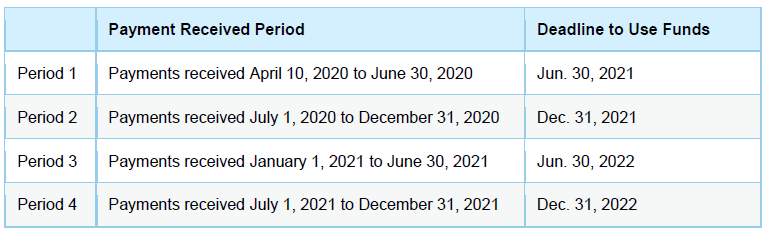
Revised Reporting Requirements and Time Periods
The PRF Reporting Portal will open for providers to start submitting information on July 1, 2021. PRF recipients must be able to demonstrate through reporting to the government that the funds were used for health care-related expenses or lost revenues attributable to COVID-19 and met all other conditions. Recipients are required to report for each Payment Received Period in which they received one or more payments exceeding, in the aggregate, $10,000. HHS will now give PRF recipients 90 days instead of 30 days to complete the required reporting.
The new reporting time periods are as follows:
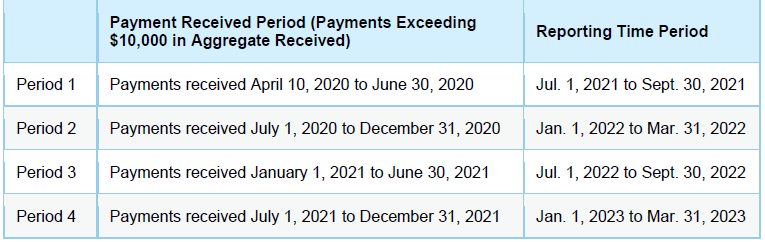
Distributions to Which These Reporting Requirements Apply
Recipients of General and Targeted Distributions, including the Skilled Nursing Facility and Nursing Home Infection Control Distribution, are required to meet these reporting requirements. However, these reporting requirements do not apply to recipients of funds from the Rural Health Clinic COVID-19 Testing Program; the Health Resources and Services Administration’s (HRSA) COVID-19 Claims Reimbursement to Health Care Providers and Facilities for Testing, Treatment, and Vaccine Administration for the Uninsured Program; or COVID-19 Coverage Assistance Fund.
More Information on PRF Reporting Requirements and Auditing
PRF recipients may access more information on federal reporting requirements and audit protocols here.
Background
The Coronavirus Aid, Relief, and Economic Security (CARES) Act, Paycheck Protection Program and Health Care Enhancement Act, and Coronavirus Response and Relief Supplemental Appropriations Act of 2021 included $178 billion in the Public Health and Social Services Emergency Fund to reimburse health care providers for health care-related expenses or lost revenues not otherwise reimbursed that are attributable to COVID-19.
The AHA last month urged HHS to extend the June 30 deadline for using the funds saying that hospitals and health systems continue to incur expenses related to COVID-19, such as ensuring an adequate workforce, acquiring equipment and supplies such as personal protective equipment, pharmaceuticals and safety equipment, and maintaining testing and additional screening for every hospital patient. “They absolutely should be able to apply their PRF funds toward these costs, which they will undoubtedly continue to incur beyond June 30 and through the end of the PHE,” AHA said in May 5 letter to HHS.
Further Questions
If you have questions, please contact AHA at 800-424-4301.

