Fact Sheet: Price Estimator Tools
The Issue
Hospitals and health systems understand the importance of sharing meaningful information that patients can use to make the best decisions for themselves and their families, including information on the cost of care. Many organizations have purchased or developed tools to assist patients in understanding the cost of their care, with a particular focus on expected out- of-pocket costs. The capability and adoption of these tools have grown rapidly over the last several years, in part due to hospitals’ ability to use these tools to fulfill one of the Hospital Price Transparency Rule provisions. Unfortunately, some policymakers want to eliminate the use of price estimator tools to meet the shoppable services requirement.
AHA Position
Price estimator tools are currently patients’ best 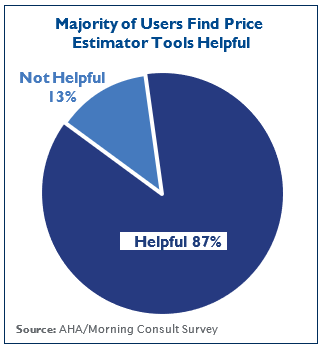 and most consumer-friendly source of information. They are more user-friendly than hospitals’ or insurers’ machine- readable files, including those that list a hospital’s shoppable services, as these can be cumbersome to navigate and will not reflect the different policies that insurers may apply to determine the final price. In addition, price estimator tools provide consumers with an estimate of their out-of-pocket costs based on their insurance benefit design, such as cost-sharing requirements and prior utilization, as well as the patient’s annual deductible. This important feature is not available from a shoppable services spreadsheet. In fact, a Morning Consult survey, conducted on behalf of the AHA to assess consumer experiences with hospital pricing information, found that patients prefer price estimator tools to shoppable services spreadsheets when estimating potential medical costs and a strong majority find them helpful in knowing where to seek medical care. Eliminating the use of price estimator tools as a method to meet the shoppable services requirement of the Hospital Price Transparency Rule would therefore reduce price transparency for patients.
and most consumer-friendly source of information. They are more user-friendly than hospitals’ or insurers’ machine- readable files, including those that list a hospital’s shoppable services, as these can be cumbersome to navigate and will not reflect the different policies that insurers may apply to determine the final price. In addition, price estimator tools provide consumers with an estimate of their out-of-pocket costs based on their insurance benefit design, such as cost-sharing requirements and prior utilization, as well as the patient’s annual deductible. This important feature is not available from a shoppable services spreadsheet. In fact, a Morning Consult survey, conducted on behalf of the AHA to assess consumer experiences with hospital pricing information, found that patients prefer price estimator tools to shoppable services spreadsheets when estimating potential medical costs and a strong majority find them helpful in knowing where to seek medical care. Eliminating the use of price estimator tools as a method to meet the shoppable services requirement of the Hospital Price Transparency Rule would therefore reduce price transparency for patients.
Background
Hospitals and health systems traditionally have relied on financial advisors — whether in person or over the phone — to help patients with inquiries about what they may pay for care. However, in recent years, many hospitals and health systems also have chosen to invest in online price estimator tools to assist patients in accessing this information for themselves.
 The growth in the use of these tools reflects changing patient expectations, improvements in technology and the ability to use these tools to meet one of the federal price transparency requirements. The widespread adoption of price estimator tools is a positive outcome for patients, as these tools are an efficient and effective way for patients to access information on their expected costs prior to care. The tools typically provide patients with estimates of both the total cost of care and the patient’s out-of-pocket costs and are usually based on real prior cases to predict the most likely course of care. They also apply the individual’s specific health insurance coverage details (e.g., copay, coinsurance, and deductible amounts).
The growth in the use of these tools reflects changing patient expectations, improvements in technology and the ability to use these tools to meet one of the federal price transparency requirements. The widespread adoption of price estimator tools is a positive outcome for patients, as these tools are an efficient and effective way for patients to access information on their expected costs prior to care. The tools typically provide patients with estimates of both the total cost of care and the patient’s out-of-pocket costs and are usually based on real prior cases to predict the most likely course of care. They also apply the individual’s specific health insurance coverage details (e.g., copay, coinsurance, and deductible amounts).
 Despite the helpful information provided by these tools, some policymakers have tried to eliminate them as a way for hospitals to adhere to the Hospital Price Transparency Rule. This could pose challenges for patients who would have to instead review a spreadsheet of shoppable services to determine their cost obligations. Insurers typically pay for a bundle of services rather than the combined total of negotiated rates for individual items or services within an episode of care. Hence, patients cannot simply add up the negotiated rates for a set of items and services using the shoppable services files. They also would need to contact their insurance company to understand the rules the insurer applies to these services, as well as learn their cost-sharing obligations and where they are in their annual out-of-pocket spending.
Despite the helpful information provided by these tools, some policymakers have tried to eliminate them as a way for hospitals to adhere to the Hospital Price Transparency Rule. This could pose challenges for patients who would have to instead review a spreadsheet of shoppable services to determine their cost obligations. Insurers typically pay for a bundle of services rather than the combined total of negotiated rates for individual items or services within an episode of care. Hence, patients cannot simply add up the negotiated rates for a set of items and services using the shoppable services files. They also would need to contact their insurance company to understand the rules the insurer applies to these services, as well as learn their cost-sharing obligations and where they are in their annual out-of-pocket spending.
 In October 2024, the AHA partnered with NORC at the University of Chicago to conduct a series of focus groups to understand the real-life experiences and needs of patients when using the hospitals’ web-based cost estimator tools compared to shoppable services files. Focus groups were conducted among 41 commercially insured adults with varying backgrounds and experiences. Participants were shown demonstrations of both hospital cost-estimator tools and shoppable services files. Compared to the spreadsheet of shoppable services files, focus group participants universally preferred the more user-friendly price estimator tools. Participants found the shoppable services files confusing and difficult to navigate. In addition, participants felt that price estimator tools more effectively provided the information they sought.
In October 2024, the AHA partnered with NORC at the University of Chicago to conduct a series of focus groups to understand the real-life experiences and needs of patients when using the hospitals’ web-based cost estimator tools compared to shoppable services files. Focus groups were conducted among 41 commercially insured adults with varying backgrounds and experiences. Participants were shown demonstrations of both hospital cost-estimator tools and shoppable services files. Compared to the spreadsheet of shoppable services files, focus group participants universally preferred the more user-friendly price estimator tools. Participants found the shoppable services files confusing and difficult to navigate. In addition, participants felt that price estimator tools more effectively provided the information they sought.
Any effort to move away from price estimator tools would do a disservice to patients, including setting back the progress made to develop meaningful price transparency options.
More information on how hospitals and health systems use price estimator tools is available on AHA’s website.


