

How AI Is Improving Diagnostics, Decision-Making and Care

Artificial intelligence (AI) holds great promise in helping health care providers gain insights and improve health outcomes. Although many questions remain regarding its safety, regulation and impact, the use of AI in clinical care is no longer in its infancy and is expected to experience exponential growth in the coming years.
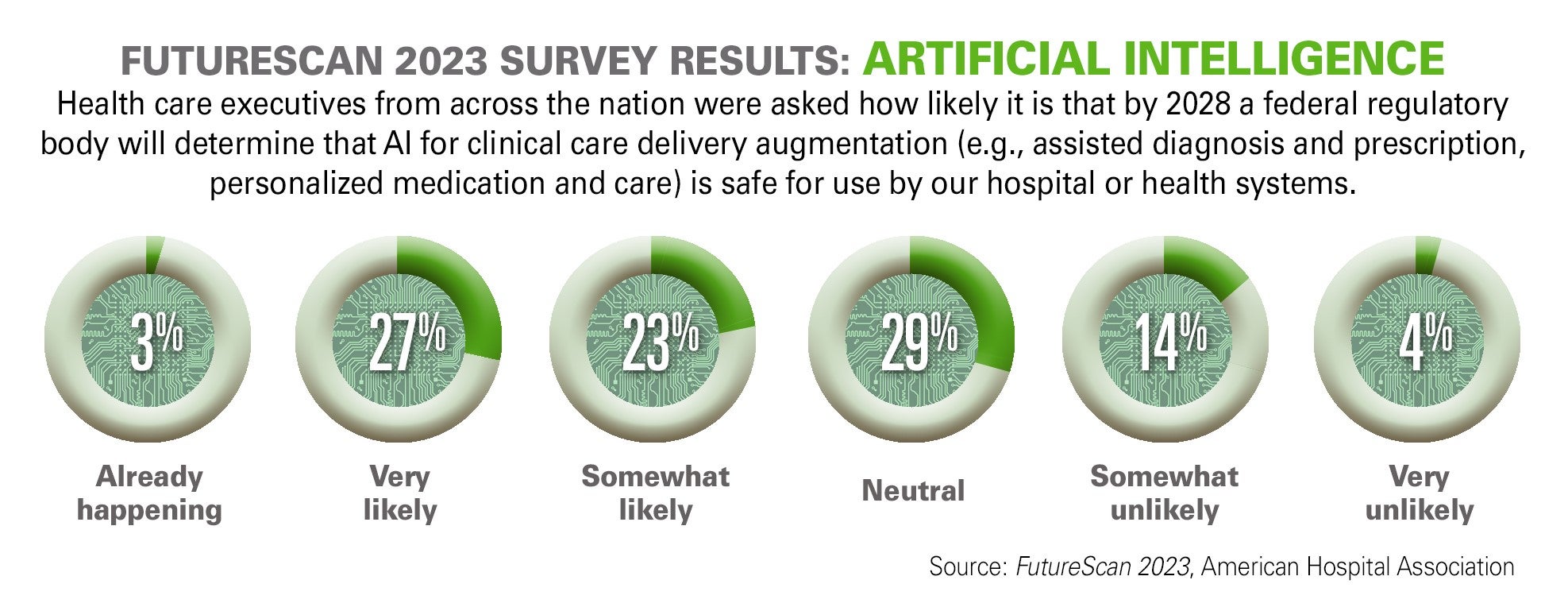
AI is improving data processing, identifying patterns and generating insights that otherwise might elude discovery from a physician’s manual effort. The next five years will be critical for hospitals and health systems to build the infrastructure needed to support AI technology, according to the recently released Futurescan 2023.
Developed by the AHA’s Society for Health Care Strategy & Market Development in collaboration with the American College of Healthcare Executives, Futurescan 2023 provides insights from thought leaders across eight topic areas, including workforce trends, health equity, the competitive environment and more. Each report is supported with data from a 2022 survey of health care leaders.
Top 3 Opportunities for AI in Clinical Care
1 | Clinical Decision Tools
One of AI’s most promising roles is in clinical decision support at the point of patient care. AI algorithms analyze a vast amount of patient data to assist medical professionals in making more informed decisions about care — outperforming traditional tools like the Modified Early Warning Score (MEWS), commonly used by hospitals to calculate the risk for clinical deterioration in a patient over the next several hours.
“While MEWS has served its purpose for a long time, and certainly did move the needle further in trying to be proactive with clinical deterioration, I think it’s pretty clear now that most of the tools that are developed using AI methods are more accurate than those bedside calculations,” said Juan Rojas, M.D., a pulmonary and critical care specialist at the University of Chicago and an expert in the application of machine learning to electronic health record data.
Rojas noted, however, that the usefulness of AI tools soon will be judged by how well they are integrated into health care systems. These complex tools require experts to monitor their use and safety, an information technology infrastructure sophisticated enough to support them and a willingness by front-line users to engage with these models.
2 | Diagnostic and Imaging
The greatest application of AI in diagnostics so far has been in imaging. “The one that’s nearest and dearest to me is AI-based assistance for lung nodule detection on CT scans, but there are similar stories around breast imaging and other areas, where AI is being used by radiologists to augment their clinical decisions,” said Rojas.
AI’s ability to recognize and process a great amount of both structured and unstructured data has led to nearly 400 Food and Drug Administration approvals of AI algorithms for the radiology field.
Hospitals today perform 3.6 billion imaging procedures annually, generating a massive amount of data. Approximately 97% of these data go unused. Machine learning allows health care professionals to structure, index and leverage this information for more accurate diagnostics.
3 | Patient Safety
The use of AI has advanced patient safety by evaluating data to produce insights, improve decision-making and optimize health outcomes. Systems that incorporate AI can improve error detection, stratify patients and manage drug delivery.
“One of the main aspirational visions is improving patient safety across the board: identifying diagnoses, problems or risks for an event earlier so that you might change the trajectory of the final outcome for the better,” Rojas said. “If you’re a radiologist using a lung nodule model and are missing early cancers, using AI will improve patient safety. The same thing goes for six-month mortality scores or other early warning signs. I would say that all the models being used in 2022 and in the next five years will be about trying to improve patient safety.”
What’s Next?
Deployment of medical AI systems in routine clinical care presents an important, yet largely unfulfilled, opportunity as the medical AI community navigates the complex ethical issues that can arise from using AI in health care. According to the Futurescan survey, more than 48% of hospital CEOs and strategy leaders are confident that by 2028, health systems will have the infrastructure in place to make use of AI in augmenting clinical decision-making.
AI is designed to enhance — not replace — traditional care delivery. Thoughtful implementation of AI offers boundless opportunities for clinical care improvements. The greatest potential for AI in the next five years is in human-centered AI design, according to Rojas.



