

AHA Testimony for the Committee on Energy and Commerce Subcommittee on Health
Testimony
of the
American Hospital Association
for the
Committee on Energy and Commerce
Subcommittee on Health
of the
U.S. House of Representatives
“Lowering Unaffordable Costs: Legislative Solutions to Increase Transparency and Competition in Health Care”
April 26, 2023
Chairman Guthrie, Ranking Member Eshoo, and members of the Subcommittee, I am Ashley Thompson, senior vice president of public policy analysis and development, at the American Hospital Association (AHA). On behalf of our nearly 5,000 member hospitals and health systems, along with our clinician partners, I appreciate the opportunity to testify today.
We appreciate the Subcommittee’s ongoing interest in addressing transparency and competition in health care. Advancing the health of our patients is a priority for the AHA and its members, whether it is providing for their health care needs or sharing the information they require to make informed care decisions.
We welcome the opportunity to discuss the legislation the Subcommittee is considering as it applies to the Hospital Price Transparency Rule; site-neutral payment policies; mergers and acquisitions; the 340B Drug Pricing Program; physician-owned hospital restrictions; and the Medicaid Disproportionate Share Hospital (DSH) Program.
Understanding the Current Environment
Our nation is facing significant health care challenges. These include an increased prevalence of chronic disease, skyrocketing demand for behavioral health care, especially among children and adolescents, sicker patients and a workforce that is struggling to continue caring for others while simultaneously addressing their own health care needs. Hospitals and health systems exist to care for our communities as well as provide a safe, meaningful place to work. Many of the underlying drivers of poor health are caused by larger societal factors that go far beyond hospitals’ walls. Yet, patients arrive at hospitals expecting for their needs to be addressed, and the nurses, doctors, technicians and other staff we rely upon are struggling to keep up with demand.
Hospitals’ and health systems’ ability to continue to serve their patients and communities is challenged by substantial resource constraints. A report released last week by the AHA details the extraordinary financial pressures continuing to affect hospitals and health systems, as well as access to patient care. The report found expenses across the board saw double digit increases in 2022 compared to pre-pandemic levels, including for workforce, drugs, medical supplies and equipment, as well as other essential operational services such as IT, sanitation, facilities management, and food and nutrition services.
Among other findings, the report showed:
- Overall hospital expenses have increased by 17.5% between 2019 and 2022. This far outpaced Medicare reimbursement, which only increased 7.5% during this same time.
- Labor costs, which on average account for about half of hospitals’ total budget, have increased 20.8% between 2019 and 2022. This is in large part due to a greater reliance on contract staffing agencies to fill workforce gaps and to meet patient demand. The outcome of this has been a staggering 258% increase in total contract labor expenses for hospitals in 2022 compared to 2019.
- For the first time in history, the median price of a new drug exceeded $200,000 — more than triple the median annual household income in the U.S. At the same time, price increases for existing drugs continue to outpace inflation, which helped drive a 19.7% increase in drug expenses per patient between 2019 and 2022.
- Hospital supply expenses per patient increased 18.5% between 2019 and 2022, outpacing increases in inflation by nearly 30%. Specifically, hospital expenses for emergency services supplies — which include ventilators, respirators and other critical equipment — experienced a nearly 33% increase during the same time period.
These factors led to the most financially challenging year for hospitals and health systems since the beginning of the COVID-19 pandemic, leaving over half of hospitals operating at a financial loss at the end of 2022, and with negative operating margins continuing into 2023.
In addition, the fiscal year (FY) 2024 Hospital Inpatient Prospective Payment System proposed rule by the Centers for Medicare & Medicaid Services (CMS) puts forward an inadequate proposed inpatient hospital payment update of 2.8%, despite hospitals incurring near decades-high inflation and increased costs for labor, equipment, drugs and supplies. The AHA has repeatedly requested that CMS and the Administration address shortcomings in its previous market basket forecasts for all hospitals. For example, CMS” inpatient payment update was a full three percentage points less than what actual market basket inflation was in 2022. These inadequate inflationary adjustments –- in addition to Medicare’s existing underpayments to hospitals –- do not reflect the economic reality in which our hospitals are providing care to our communities.
Workforce challenges also are taking a significant toll on hospitals and health systems. Long building structural changes in the health care workforce, combined with the profound impact of the COVID-19 pandemic, have left hospitals and health systems facing a national staffing emergency that is jeopardizing patient access to care. Patients requiring additional care after a hospitalization –- such as skilled nursing, behavioral health or therapy-at-home — face growing delays in accessing those services due to personnel shortages. These delays also put incredible strain on hospitals and health systems, as they must bear the costs of caring for patients during these excess days without appropriate reimbursement, and they add burden on an already stretched workforce.
The shortages have been challenging for acute care hospitals as well as post-acute care and other providers receiving patient transfers from acute care hospitals, such as psychiatric hospitals. As a result, post-acute care and other providers have been unable to accept new patients, creating patient bottlenecks at acute care hospitals. Rehabilitation and long-term care hospitals also report similar patient bottlenecks, with difficulties discharging their patients to other post-acute care providers, such as skilled nursing facilities.
Hospital Price Transparency Rule
Hospitals and health systems are committed to empowering patients with all the information they need to live their healthiest lives. This includes ensuring they have access to accurate price information when seeking care. Hospitals and health systems are working to comply with both state and federal price transparency policies, which are varied and sometimes conflicting. At the federal level, these include the Hospital Price Transparency Rule. As of Jan. 1, 2021, hospitals are required to publicly post via machine-readable files five different “standard charges”: gross charges; payer-specific negotiated rates; de-identified minimum and maximum negotiated rates; and discounted cash prices. The rule also requires hospitals to provide patients with an out-of-pocket cost estimator tool or payer-specific negotiated rates for at least 300 shoppable services.
CMS has a process in place to ensure hospital compliance with the Hospital Price Transparency Rule. This includes a review, usually involving direct discourse with the hospitals; if deficiencies are identified, a warning letter is sent from the agency; and if the deficiencies are not corrected, a corrective action plan is requested. Should a hospital continue to fail to come into compliance, CMS then applies a civil monetary penalty.
CMS found that in 2022, 70% of hospitals complied with both components of the Hospital Price Transparency Rule, including the consumer-friendly display of shoppable services information, as well as the machine-readable file requirements. This is an increase from 27% in 2021. Moreover, when looking at each individual component of the rule, 82% of hospitals met the consumer-friendly display of shoppable services information requirement in 2022 (up from 66% in 2021) and 82% met the machine-readable file requirement (up from 30% in 2021).
These numbers show significant progress on the part of hospitals and health systems — while acknowledging the work that remains — in implementing these requirements. The lower compliance rate in 2021, however, should not be interpreted as a lack of hospital commitment to transparency. Instead, it reflects the incredible challenges hospitals were experiencing in 2020 and 2021 in addressing the most acute phases of the COVID-19 public health emergency, which strained hospitals’ staff and required the diversion of personnel and financial resources. As the pandemic phase of COVID-19 winds down and hospitals have been able to resume more standard operations, they are able to dedicate the resources necessary to build the full suite of price transparency tools.
CMS also shared information regarding how it has interacted with hospitals to support compliance and the issuance of penalties:
“As of January 2023, CMS had issued nearly 500 warning notices and over 230 requests for corrective action plans since the initial implementing regulation went into effect in 2021. Nearly 300 hospitals have addressed problems and have become compliant with the regulations, leading to closure of their cases. While it was necessary to issue penalties to two hospitals in 2022 for noncompliance (posted on the CMS website), every other hospital that was reviewed has corrected its deficiencies.”
Unfortunately, some third parties continue to issue reports mischaracterizing whether hospitals are complying with the Hospital Price Transparency Rule, as was detailed in a letter AHA sent recently to House Energy and Commerce Chair Rodgers and Ranking Member Pallone. These reports fail to acknowledge CMS’ requirements, such as how to fill in an individual negotiated rate when such a rate does not exist due to patient services being bundled and billed together. In this instance, CMS has said a blank cell would be appropriate since there is no negotiated rate to include. Despite this, some outside groups still count any file with blank cells as “noncompliant.” This fundamental misrepresentation of the rules has only served to advance misinformation and confusion on the issue and distract from genuine productive discussions and efforts around what patients want in terms of transparency data and how best to provide that information.
In addition to the CMS report on compliance, we would draw your attention to a recent report from Turquoise Health that found about 84% of hospitals had posted a machine-readable file containing rate information by the end of first-quarter 2023, up from 65% the previous quarter.
Recommendations
Hospitals and health systems are eager to continue working toward providing the best possible price estimates for their patients. We ask Congress and the Administration to take the following steps to support these efforts, including:
- Review and streamline the existing transparency policies with a priority objective of reducing potential patient confusion and unnecessary regulatory burden on providers;
- Continue to convene patients, providers and payers to seek input on how to make federal price transparency policies as patient-centered as possible; and
- Refrain from advancing additional legislation or regulations that may further confuse or complicate providers’ ability to provide meaningful price estimates while adding unnecessary costs to the health care system.
Medicare Outpatient Site-Neutral Payment Reductions
The AHA strongly opposes additional site-neutral payment cuts, which threaten access to care, especially in rural and historically marginalized communities. Existing site-neutral payment policies have already had a significantly negative impact on the financial sustainability of hospitals and health systems, particularly as they continue to manage the aftermath of the COVID-19 pandemic as well as the challenges posed by workforce shortages, broken supply chains and historic levels of inflation that have increased the costs of caring for patients. Such policies have contributed to Medicare’s chronic failure to cover the cost of caring for its beneficiaries, putting a strain on hospitals’ ability to continue to care for their communities. Further cuts would only exacerbate this shortfall and may cause hospitals to significantly reduce services or close altogether.
Site-neutral policies also fail to account for the fundamental differences between hospital outpatient departments (HOPDs) and other sites of care. The cost of care delivered in hospitals and health systems takes into account the unique benefits that they provide to their communities. This includes the investments made to maintain standby capacity for natural and man-made disasters, public health emergencies and unexpected traumatic events, as well as deliver 24/7 emergency care to all who come to the hospital, regardless of ability to pay or insurance status. Hospitals and health systems provide access to critical services and programs that may not be otherwise available, especially in low-income and rural communities.
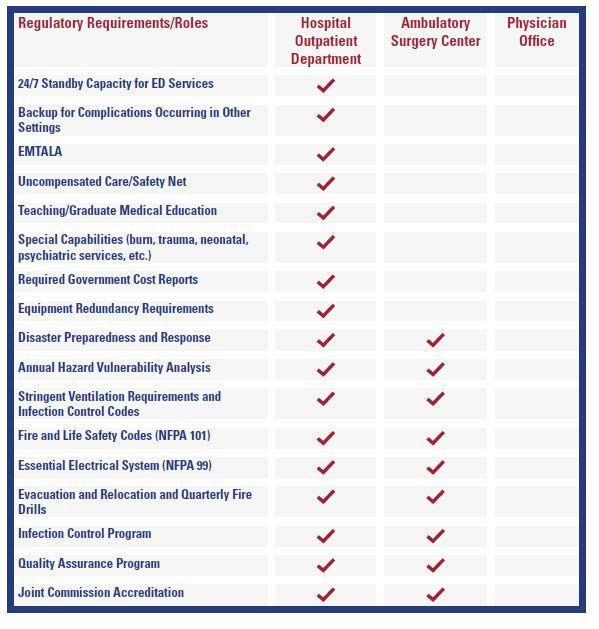
Hospital facilities also treat patients who are sicker and have more chronic conditions than those treated in physician offices or ambulatory surgical centers, which requires a greater use of resources. In addition, hospital facilities must comply with a much more comprehensive scope of licensing, accreditation and other regulatory requirements compared to other sites of care, such as ambulatory surgery centers (ASCs) and physician offices (see chart below).
Specifically, physicians often refer sicker patients with higher-risk conditions to hospital-based settings for safety reasons, as hospitals are better equipped to handle complications and emergencies, which often require the use of additional resources that other settings do not typically provide. Indeed, nearly half of all Medicare beneficiaries live with four or more chronic conditions and one-third have one or more limitations in activities of daily living (ADL). Compared to independent physician offices and ASCs, data1 show that, on average, HOPDs treat Medicare patients who are suffering from more severe chronic conditions and have higher prior utilization of hospitals and emergency departments. Such co-morbid conditions may include morbidly obese patients, patients with mental health issues, such as dementia, and disabled patients. Because some co-morbid conditions can make even simple procedures more dangerous and increase the likelihood of complications, it is prudent to utilize the greater capacities and capabilities of HOPDs to assist patients if something goes wrong during a procedure. In fact, patients experiencing unexpected life or limb-threatening complications in physician offices and ASCs are usually emergently transferred to the closest hospital via an ambulance.
Many such examples exist in which less healthy patients are, for clinical and safety reasons, referred to HOPDs rather than other settings. This includes diagnostic cardiac catheterization procedures, which sometimes reveal blockages in the coronary arteries and require immediate interventions that cannot be safely provided in an ASC or physician office. Another example is total knee arthroplasty (TKA) procedures. While these services often can be successfully performed for healthier Medicare patients in an ASC setting, it is not appropriate for others in the Medicare population who have co-morbid conditions and ADL limitations. For instance, patients undergoing TKA are at increased risk of myocardial infarction (with patients 80 years or older at highest risk) and deep vein thrombosis with the potential to propagate a potentially lethal pulmonary embolus.
Moreover, according to the Medicare Payment Advisory Commission (MedPAC), for the past 20 years, Medicare payments have failed to cover the costs of caring for Medicare beneficiaries. This underpayment is due in part to existing site-neutral payment policies that have substantially cut reimbursements; further site-neutral cuts would only exacerbate this gap. According to MedPAC, overall Medicare hospital margins were -6.3% in 2021 after accounting for temporary COVID-19 relief funds. Without these temporary relief funds, the overall Medicare margin for 2021 remained depressed at -8.2% after hitting a staggering low of -12.3% in 2020. Indeed, on average, Medicare only pays 84 cents for every dollar hospitals spend providing care to Medicare beneficiaries. Moreover, overall median hospital operating margins were negative throughout 2022 and into the beginning of 2023. Site-neutral cuts have already contributed to these shortfalls, and any further expansion of these policies will threaten patients’ access to quality care.
It is important to understand that site-neutral policies generally rely upon an assumption that Medicare’s physician fee schedule rates are fair and accurate. They are not. The physician fee schedule “conversion factor” in 2023 is almost $3 less than it was 25 years ago, in 1998. This is even without considering inflation. In addition to inadequate reimbursement, physicians, and the entire health care workforce writ large, are grappling with physical and emotional strain, burnout and shortages. They are facing enormous challenges, including skyrocketing administrative and regulatory burden in the form of, for example, electronic health record requirements, and increasing violence in their workplace, not to mention the once-in-a-lifetime pandemic that brought the entire health care system to the brink of collapse. As a result, our members report that physicians in their community regularly express the sentiment that their freestanding practices are no longer viable. And, rather than allow their communities to go without this critical care, hospitals acquire the practice in order to maintain patient access.
Now more than ever, hospitals need stable and adequate reimbursements as they face challenging financial circumstances. Expanding site-neutral cuts to additional HOPDs would endanger the critical role that HOPDs play in their communities, including access to care for patients, especially the most medically complex.
Hospital Mergers and Acquisitions
Mergers and acquisitions are one of the most important tools that some hospitals use to increase access, provide quality care and manage financial pressures and risk. These partnerships enable hospitals to expand service offerings, broaden networks and access to specialists, improve quality and better serve patients where they live. They also provide scale to help reduce costs associated with obtaining medical services, supplies and prescription drugs, and enable health systems to reduce other operational costs. Ultimately, hospital mergers and acquisitions expand and preserve access to care.
Emerging research has demonstrated a clear association between consolidation and quality improvement. For example, one study found that a full-integration approach is associated with improvements in mortality and readmission rates, among other quality and outcome improvements.2 Another study found significant reductions in mortality for a number of common conditions — including acute myocardial infarction, heart failure, acute stroke and pneumonia — among patients at rural hospitals that had merged or been acquired.3 Being part of a system also can help hospitals comply with new, resource-intensive regulatory requirements. For example, hospitals affiliated with systems are more likely to have a price transparency score of 5 out of 5 stars, according to a recent report by Turquoise Heath.
Mergers and acquisitions help hospitals improve access to care by expanding the types of specialists and services available to patients. According to an analysis by Kaufman Hall, nearly 40% of affiliated hospitals added one or more services post-acquisition. Mergers and acquisitions also are a vital tool that some health systems use to keep financially struggling hospitals open, thereby averting bankruptcy or even closure.4 When hospitals become part of a health system, the continuum of care is strengthened for patients and the community, resulting in better care and decreased readmission rates.
Mergers and acquisitions also have played a critical role in preserving access to care in rural areas. An AHA analysis of the UNC Sheps Center data on rural hospital closures between 2010 and 2020 shows that slightly more than half of the hospitals that closed were independent. Health systems typically acquire rural hospitals when these hospitals are under financial distress. Research has shown that rural hospitals are less likely to close after acquisition compared to independent hospitals and that mergers have improved access and quality of care for rural hospitals.5 Acquired hospitals typically form new collaborations or partnerships with larger health systems, which promotes access to specialists, telehealth and other care for rural patients.6
340B Drug Pricing Program
The 340B Drug Pricing Program allows hospitals to stretch limited federal resources to reduce the price of outpatient pharmaceuticals for patients as well as expand health services to the patients and communities they serve. 340B hospitals achieve savings by purchasing drugs at a discount. The amount of that discount depends on drug companies’ pricing decisions, with the discount increasing the more the drug companies decide to raise the price of their drugs. The Health Resources and Services Administration (HRSA) estimates that the average discount is anywhere between 25% to 50%.
Hospitals use 340B savings to provide a range of vital programs and services, which include, but are not limited to, the provision of free or discounted drugs to low-income patients, free care for uninsured patients and support for behavioral health clinics and community health programs. In fact, in the most recent year for which information is available, tax-exempt 340B hospitals provided nearly $68 billion in total benefits to their communities. This program is particularly important as drug prices continue to rise and hospitals face increased inflationary cost pressures across all their supplies and services. The AHA urges Congress to continue to protect this critical program and oppose efforts to further restrict eligibility, which would result in reduced access to quality care for the patients and communities served by 340B hospitals.
We appreciate the Subcommittee’s support for the 340B program and interest in making certain all stakeholders meet the 340BB program integrity requirements. 340B hospitals must annually recertify their eligibility to participate and attest to meeting all the program requirements; participate in audits conducted by HRSA and drug manufacturers; and maintain auditable records and inventories of all 340B and non-340B prescription drugs. The AHA is working with its 340B member hospitals, through the AHA Good Stewardship Principles, on efforts to strengthen the 340B program by helping 340B hospitals support greater transparency in communicating publicly the immense value the program brings to patients and communities.
However, the AHA would oppose efforts to create significant new reporting requirements for 340B hospitals that do not reflect the true value or intent of the 340B program. Reporting on a drug’s reimbursement amount would not provide relevant information because the reimbursement amount is the same for 340B hospitals and non-340B hospitals alike. 340B savings for a hospital are based on the difference between what the hospital paid to acquire the drug under 340B versus what the hospital would have paid to acquire the drug outside of the 340B program. Focusing on these measures and hospitals’ charity care numbers alone would not provide policy makers with an accurate picture of the myriad benefits the patients and communities receive due to a hospitals’ participation in the 340B program. 340B hospitals are committed to transparency, but believe transparency should involve mutual concessions. Any measures that increase transparency for 340B providers also should include greater transparency for drug companies, including how they set their prices and how much they decide to increase their prices.
As part of any effort to make changes to the 340B program, the AHA encourages Congress to address the alarming efforts by some drug companies’ to restrict access to 340B discounted drugs for 340B hospitals that have established community and specialty pharmacy arrangements. Since October 2022, over 20 drug companies have adopted these restrictive policies to the severe detriment of 340B hospitals and their patients. The financial impact on 340B hospitals is significant. For 340B critical access hospitals, AHA’s survey reports average annual losses of over $500,000 and 340B disproportionate share hospitals have average annual losses of nearly $3 million. The AHA continues to actively support HRSA in its efforts to enforce the requirements for drug companies set forth in the 340B statute.
Restrictions on Physician-Owned Hospitals
America’s community hospitals and health systems welcome fair competition, where health care entities can compete based on quality, price, safety and patient satisfaction. But physician-owned hospitals (POH) — where physicians cherry-pick the healthiest and best-insured patients and self-refer those patients to facilities in which they have an ownership interest — represent the antithesis of competition. The AHA strongly opposes any changes that would either expand the number of POHs or ease restrictions on the growth of existing facilities.
Congress acted in 2010 to close the “whole hospital” loophole in the Stark law and placed restrictions on POHs. That provision represented a carefully crafted compromise to protect hospitals with a Medicare provider number as of Dec. 31, 2010 and allow those facilities to expand when increased hospital capacity is needed. Since 2010, eight POHs have applied for the exceptions process and have been allowed to expand.
Several analyses, including by the Congressional Budget Office, MedPAC and independent researchers, have concluded that physician self-referral leads to greater per capita utilization of services and higher costs for the Medicare program. In fact, according to the Congressional Budget Office, closing the “whole hospital” exception loophole in the Stark law reduced the federal deficit by $500 million over 10 years. Bills that would repeal the 2010 law would erase those savings and increase the federal deficit.
Furthermore, POHs tend to cherry-pick the most profitable patients and services, jeopardizing communities’ access to full-service hospital care. The Government Accountability Office, CMS and MedPAC have found that patients in POHs tend to be healthier than patients with the same diagnoses who are taken care of by community hospitals. This practice of self-referring physicians carefully selecting their patients creates a destabilizing environment that leaves sicker and less-affluent patients to community hospitals, thereby placing these hospitals at a distinct financial disadvantage. This is because community hospitals rely on cross-subsidies from those services targeted by POHs to support essential, but under-reimbursed, services such as emergency, trauma and burn care. By siphoning off the most profitable services and patients, POHs threaten the ability of community hospitals to offer quality, comprehensive care and serve as the health care provider for all patients, regardless of income or insurance status, in their communities.
Medicaid DSH Program
Congress established the Medicaid DSH program to provide financial assistance to hospitals serving a disproportionate number of low-income patients to ensure Medicaid and uninsured patients have access to health care services. These hospitals also provide critical community services, such as trauma and burn care, maternal and child health care, high-risk neonatal care and disaster preparedness resources. The patients they serve are among those that need care the most and often experience challenges accessing it, including children, the poor, the disabled and the elderly.
Reductions to the Medicaid DSH program were enacted as part of the Affordable Care Act, with the reasoning that hospitals would have less uncompensated care as health insurance coverage increased. Under current statute, the Medicaid DSH cut is $8 billion for each of the next four fiscal years (2024-2027, for a total of $32 billion for all four years).
Unfortunately, the projected coverage levels have not been realized and hospitals continue to care for patients for whom they are not receiving payment. The redetermination process that began on April 1 also may lead to additional individuals becoming uninsured as states decide who remains eligible for the Medicaid program. In addition, hospitals are dealing with financial instability due to the long-lasting impact of the COVID-19 pandemic as well as the increased inflationary costs they have incurred for the staffing, supplies, drugs and equipment necessary to be able to serve their communities.
Consequently, the need for the Medicaid DSH payments is still vital for the hospitals that rely on the program. Congress has, with bipartisan support, prevented the cuts from going into effect previously. The AHA supports efforts to once again address the Medicaid DSH reductions.
Conclusion
We thank you for the opportunity to share the hospital and health system field’s perspective and appreciate that these topics are priority areas for the Subcommittee, as they are for our field and our patients. We look forward to continuing to work with you to address these important issues.
- https://www.aha.org/system/files/media/file/2023/03/Comparison-of-Medicare-Beneficiary-Characteristics-Between-Hospital-Outpatient-Departments-and-Other-Ambulatory-Care-Settings.pdf
- https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2787652
- https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2784342
- https://www.aha.org/system/files/media/file/2021/10/KH-AHA-Benefits-of-Hospital-Mergers-Acquisitions-2021-10-08.pdf
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9250050/
- https://www.aha.org/system/files/media/file/2021/10/KH-AHA-Benefits-of-Hospital-Mergers-Acquisitions-2021-10-08.pdf


