

Assessing the Changing Face of Strategic Partnerships

The path to long-term sustainability and relevance for health care organizations is littered with challenges and obstacles that make strategic planning ever more difficult in the face of mounting market disruption. A key indicator to future success will be how quickly and effectively provider organizations can pursue impactful and strategic collaborations both inside and outside the provider world, notes Ninfa M. Saunders, president and CEO of Georgia-based Navicent Health, an Atrium Health system.
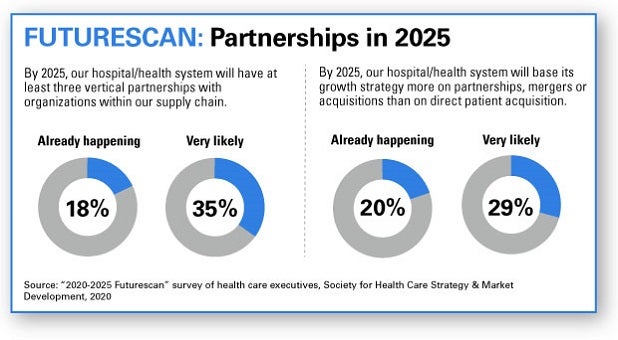
So, how is the field faring on collaboration with fellow providers and outside partnerships? Better than many might think. The latest national “Futurescan” survey of health care executives found that 18% of respondents already have entered into at least three vertical partnerships with organizations in areas such as insurers and pharmaceutical companies, and another 63% are somewhat or very likely to do so within the next five years.
Produced by the AHA’s Society for Health Care Strategy & Market Development, “Futurescan 2020-2025: Health Care Trends and Implications” explores key forces that are transforming health care in disruptive innovation, technologies that are reshaping the future of medicine and the impact of new entrants on the future of health care.
In her comments in the Changing Face of Strategic Health Care Partnerships section, Saunders provides examples of various types of transformational partnerships. Among them:
- Brand/expertise extension: Mayo Clinic Network offers providers the chance to join after a comprehensive evaluation process. Once accepted, physicians can share Mayo’s branding and expertise while still retaining autonomy.
- Joint venture: Vivity, is a narrow-network health plan that involved a joint venture between Anthem Blue Cross and seven health systems in Southern California, all of which share risk.
- Management services agreement: Novant Health’s shared services division offers a variety of products to community hospitals, including management of supply chain/purchasing, revenue cycle, clinical equipment and service lines.
Other nontraditional and innovative partnership models include collaborating with local groups to address public health issues and direct contracting with employers to provide medical services to their employees and are becoming essential to provider organizations as they address challenges. Hospitals and health systems will need to evaluate these models carefully to determine the approach and structure that are best suited to their needs.
Saunders says each partnership must support the organization’s enterprise strategic plan and at least one of its four guiding strategic objectives: (1) engage consumers/patients in meaningful ways, (2) create healthy communities, (3) demonstrate value by taking on risk and (4) leverage disruptive technologies effectively.
At Navicent Health Saunders and her team have developed nontraditional partnerships with startups and health care companies. These partnerships address issues like community health, health disparities, access to care, resources and distributed care. Navicent has several horizontal partnerships, including one with Atrium Health to ensure health equity, access and affordability by addressing patient and community needs across a large area of the Southeast.
Navicent also has a vertical partnership with SynsorMed, a digital health platform company, to embed the early-stage startup’s technical team with Navicent’s respiratory therapists and community workers. Its focus is to close health disparity gaps in populations of patients with chronic obstructive pulmonary disease.
Saunders advises leaders to seize the opportunity to create new, innovative and impactful partnerships that challenge the status quo. “Partnerships may be the only way we can successfully disrupt a health care system that is in dire need of change,” she says.
The “Futurescan 2020-2025” report is free to SHSMD members. You can also register for the February 5, 2020, webinar "Futurescan 2020-2025 Insights: Transformation and Disruption."



