

Team-Based Care Can Add Value, Improve Outcomes in Pandemic Response
 With the flu season upon us and indications surfacing of a COVID-19 resurgence in many regions of the country, hospitals and health systems will need a well-coordinated clinical response to manage the impact on front-line caregivers. Many are turning to team-based models of care that encompass patients’ medical and social needs across the care continuum.
With the flu season upon us and indications surfacing of a COVID-19 resurgence in many regions of the country, hospitals and health systems will need a well-coordinated clinical response to manage the impact on front-line caregivers. Many are turning to team-based models of care that encompass patients’ medical and social needs across the care continuum.
A new issue brief from AHA, “Team-based Care Creates Value,” examines this low-tech approach that allows health care workers from various professional disciplines to provide customized, patient-centered care to manage the physical, psychological and spiritual needs of patients.
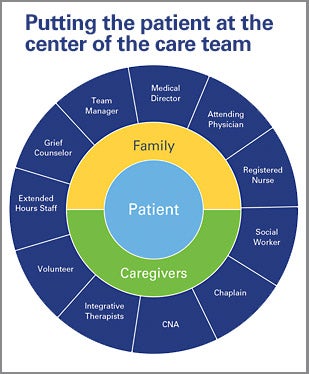 The report explores how to build effective care teams and how organizations can use team-based models to create value by improving outcomes, enhancing the patient experience and reducing cost. Teams that communicate effectively and demonstrate mutual support reduce the potential for error, resulting in enhanced patient safety and improved clinical performance.
The report explores how to build effective care teams and how organizations can use team-based models to create value by improving outcomes, enhancing the patient experience and reducing cost. Teams that communicate effectively and demonstrate mutual support reduce the potential for error, resulting in enhanced patient safety and improved clinical performance.
In one team-based care model, Virginia-based Clinch Valley Medical Center partnered with the Appalachian Agency for Senior Citizens, a nonprofit group that works to improve the lives of seniors, to reduce readmissions and emergency department visits. A core team from CVMC and AASC, including case workers, pharmacists, respiratory therapists and representatives from administration and a primary care clinic, make home visits to recently discharged patients to address upstream health issues and social determinants of health that may hinder patients’ recovery and well-being. At any one time, the team tracks the needs of approximately 15-22 patients with comorbidities and complex health issues, texting each other to provide services when concerns arise. The team has reduced avoidable readmissions from 11.8% to 7.8% and reduced costs for consumers.
Additional resources on team-based care are also available. The AHA has produced “TeamSTEPPS Video Training for the COVID-19 Crisis,” a new limited video series featuring TeamSTEPPS tools designed to optimize teamwork and communication, two skill sets that are especially needed during the pandemic. Each video focuses on how different TeamSTEPPS tools can be used in COVID-19 scenarios.



