Fact Sheet: Rural Community Hospital (RCH) Demonstration
The Issue
The Rural Community Hospital (RCH) demonstration tests an alternative payment model for small rural hospitals, in response to concerns that they face financial difficulties with Medicare’s inpatient prospective payment system (IPPS). In particular, the demonstration focuses on hospitals that may lack economies of scale but are too large to be critical access hospitals (CAHs) and therefore cannot receive cost-based reimbursement for services provided to Medicare beneficiaries. Rural hospitals are the cornerstones of their communities; they provide access to care close to home, employment opportunities and support of the local economy. However, many of these hospitals struggle to address the increasing challenges of providing health care in rural America, including low patient volumes, sicker patient populations, geographic isolation, shifts in care delivery, increased regulatory burden and the opioid crisis. More information on the challenges that rural hospitals face can be found in the AHA’s Rural Report.
Background
The RCH program tests reasonable cost reimbursement for inpatient services in rural hospitals that have fewer than 51 acute-care beds, provide 24-hour emergency care services, and are not designated or eligible for designation as a CAH. RCHs receive payment for inpatient services, including swing bed services, based on the following rules1:
 First (base) year: RCH is paid reasonable costs of providing covered inpatient services.
First (base) year: RCH is paid reasonable costs of providing covered inpatient services.- Second and subsequent years: RCH is paid the lesser of their reasonable costs or a target amount.
- Second year: Target amount is the base
year’s reasonable costs, plus the IPPS
update factor. - Subsequent years: Target amount is the
prior year’s target amount, plus the IPPS
update factor.
- Second year: Target amount is the base
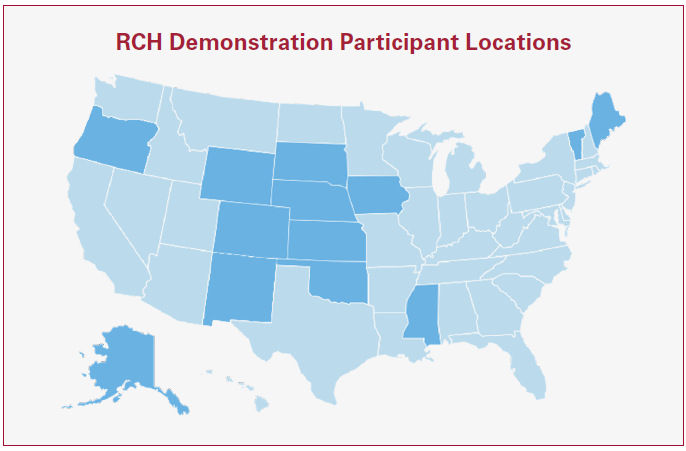
The program was initially authorized by the Medicare Prescription Drug, Improvement, and Modernization Act of 2003 and was most recently extended for another five-year period in 2020. The Center for Medicare & Medicaid Services selected 10 new hospitals to join the demonstration project in April 2025. Hospitals located in one of the 20 states with the lowest population densities are prioritized for participation. Historically, the target amount has been adjusted for case mix. No more than 30 hospitals are allowed by law to participate in the RCH demonstration. Current participants are located in AK, CO, IA, KS, ME, MS, NE, NM, OK, OR, SD, VT and WY. By statute, the RCH program is budget-neutral in the IPPS. Some RCH participants have already been forced to exit the program because the end date of the current five-year term is staggered. If not further extended, the program will completely end on June 30, 2028. Hospitals whose five-year term has already expired will receive retroactive payments if the demo is extended.
The September 2025 evaluation of the RCH program provides further evidence to support the model’s success.2 Overall, RCHs have reported that participating in the demonstration has allowed them to continue providing care in their communities; prevented them from having to make dramatic alterations in their operations; and facilitated their continued support of their local economies. These improvements were made possible because of the financial benefits from participating in the model.
AHA Take
Congress should pass the Rural Community Hospital Demonstration Program Reauthorization Act (S. 4460 / H.R. 8967) to extend the RCH program for an additional five years.
End notes
- Includes operating and capital costs, as well as bad debt.
- For more details on how financial conditions varied by hospital market area, please see the Rural Community Hospital Demonstration Report to Congress.


