
Data-Driven Initiative Drives Down Disparities in Rural Health Care
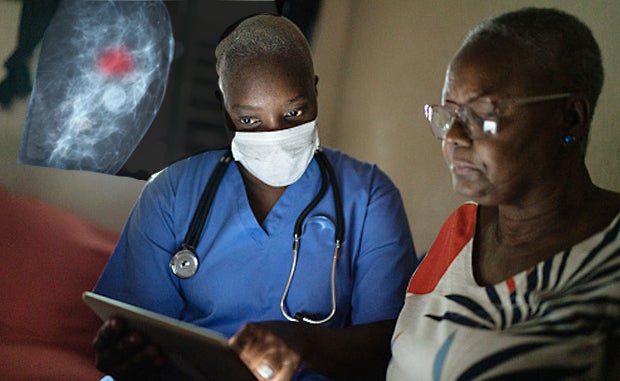
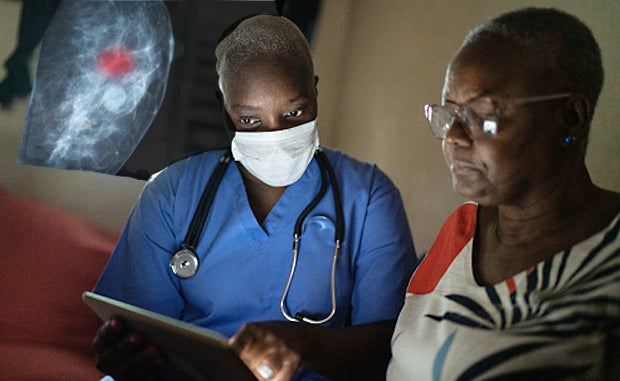
Identifying the underlying factors that contribute to disparities in outcomes in vulnerable rural populations and developing strategies to address these issues remain constant challenges, but progress is being made. OSF Healthcare’s Health Equities Action Lab (HEAL) is employing a data-driven strategy to address breast cancer disparity outcomes among its Illinois patients, 65% of whom live in rural areas.
Specifically, the Illinois-based, 14-hospital nonprofit health system has set out to uncover and better understand the factors that contribute to a 60% higher mortality rate for Black vs. white women aged 45 to 69 who develop breast cancer, while designing strategies to more effectively reach, educate and motivate women who haven’t had a mammogram in two years or more to be screened.
Speaking at the recent AHA Rural Health Care Leadership Conference, Sarah Stewart de Ramirez, M.D., MPH, vice president and chief medical officer of clinical innovation at OSF, outlined her system’s multilevel approach to analyzing data and giving community health workers the digital means to help improve access to care and reduce disparities in outcomes.
 OSF’s analysis of national, state and county-level data found that the long-held belief in the clinical community that genetic susceptibility largely accounts for the disparity levels in higher cancer rates for Black women wasn’t adequate. A deeper look at the data and clinical studies revealed that genetics only accounts for about 20% of the disparity in breast cancer mortality among women. The remaining disparity, borne out by multiple studies, is substantiated by social and structural determinants of health, which have been measured throughout the cycle — from screening to biopsy, diagnosis, treatment and survival.
OSF’s analysis of national, state and county-level data found that the long-held belief in the clinical community that genetic susceptibility largely accounts for the disparity levels in higher cancer rates for Black women wasn’t adequate. A deeper look at the data and clinical studies revealed that genetics only accounts for about 20% of the disparity in breast cancer mortality among women. The remaining disparity, borne out by multiple studies, is substantiated by social and structural determinants of health, which have been measured throughout the cycle — from screening to biopsy, diagnosis, treatment and survival.
With this knowledge, the team went back to the beginning of the process — mammography screening — and examined data on race and income. The data indicated mammography income-driven disparities of 15% to 25% across all OSF counties. With help from a grant funded by BlueCross BlueShield of Illinois and executed with a partnership of the AHA’s Institute for Diversity and Health Equity, OSF set goals and developed action plans to create demand and increase access to mammography services in vulnerable populations.
OSF designed three interventions with its grant:
Sending Text Alerts
These messages, aimed at women who have not had a mammogram in more than two years, urges them to schedule their screening because they are overdue. Links are provided in the texts to direct patients to an OSF microsite where they can self-schedule, view digital and video education and chat with a digital health care worker who can answer their questions.
Calling Patients
Digital health care workers call patients to schedule video or phone visits to provide education about the mammogram process, assist with scheduling and to screen for social determinants. They also can link patients with cancer navigators and social workers who can help them overcome barriers to care.
Engaging in Community Outreach
OSF has developed targeted outreach through community events where women can get walk-in mammograms, lung cancer screenings and receive health education.
Early returns from these efforts show progress. For example:
- 88% of the more than 3,300 texts sent reached a working cellphone, with only 38 recipients opting out.
- 58% of those who received texts went to the microsite to access education.
- 294 mammograms have been scheduled online since the program launched.
On-demand access to the AHA Rural Health Care Leadership Conference sessions will be available for purchase by new registrants beginning Feb. 26. Register here.
For more on how to improve health equity, consult these AHA resources:



