

Preparing For Behavioral Health’s Future

COVID-19 and the economic woes that followed have combined to put an enormous strain on society’s behavioral health. Indeed, the global pandemic has accentuated the need for more behavioral health services across all socio-economic sectors.
The pandemic also brought massive disruption to the field. Hospitals and health systems rapidly scaled remote care platforms to increase access to care. Employers increasingly reached out to educate and encourage employees to seek help when needed, and both public and private insurers changed reimbursement policies for remote care. So what does the future hold?
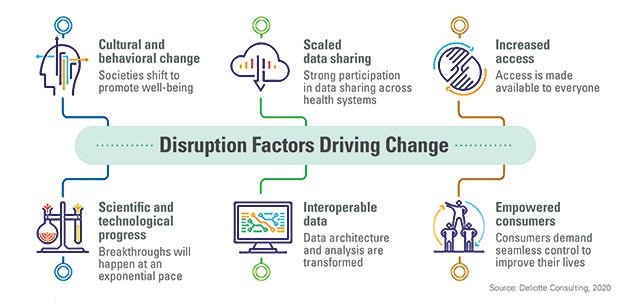
In its recent “Future of Behavioral Health” report, Deloitte notes that six disruption factors will drive behavioral health’s future:
- Cultural changes will lessen the stigma associated with behavioral health and, instead, promote well-being.
- Scaled data sharing across health systems will allow for proactive identification and treatment of behavioral health conditions.
- Scientific breakthroughs and technology advances will increase the number of effective treatments.
- Interoperable data will support the sharing of diverse data types to tailor treatments thanks to a better understanding of each individual’s behavioral health situation.
- Empowered consumers will demand seamless control of their care to improve their lives.
- In combination, these factors should provide increased access for all patients.
Leaning Heavily on Analytics
Providers have the opportunity to build on these disruption factors to deliver personalized care, Deloitte notes.
Providers will have to access consumer behavioral health data and have the ability to apply advanced analytics and artificial intelligence to enable preventive interventions, predict early onset of behavioral disorders, recommend interventions to improve behavioral health outcomes and tailor solutions for complex behavioral health conditions.
Emerging technologies — from self-guided, gamified treatment to virtual assistants and artificial intelligence — could be used throughout the care process. Enhanced digital triage processes, augmented and virtual reality treatments, and computational psychiatry also could complement traditional care delivery, Deloitte argues.
As providers sift through technologies to supplement care delivery, AHA’s Behavioral Digital Pulse can help hospitals and health systems learn where existing capabilities can support scaling digital transformation. With this member benefit, participants can benchmark their digital capabilities against other leaders in the field and learn which tools are fueling success.
Building Workforce Capacity
Potential high-tech solutions only go so far, however. Providers will need to augment workforce capacity through community and in-home care to ensure that patients receive treatment in the right place and time. Physicians of all specialties will simultaneously need to integrate preventive behavioral treatment into care models. Integrating primary care and behavioral health is another critical step toward treating the whole patient, as conveyed in an AHA Market Insights report.
These efforts will require creative workforce planning and tailored education. Providers also need to continue focusing on value-based financing models that compensate providers for integrated physical and behavioral health care that is quality driven. This shift should allow providers to invest in the preventive care required for behavioral health, mitigating any downstream financial consequences for earlier intervention.
Make no mistake, enormous challenges will come with efforts to implement a new culture that aligns workforce incentives with organizational goals, the report concludes. Nurturing collaborative relationships with insurers and aligning goals to address behavioral health will be vital to success.



