

Houston Methodist’s Digital-First Mindset Fuels Transformation
 At the height of the pandemic, the clinical care pathways team at Houston Methodist received a message from an incredulous surgical patient. The individual received targeted messages to their phone about what to expect before and after the operation.
At the height of the pandemic, the clinical care pathways team at Houston Methodist received a message from an incredulous surgical patient. The individual received targeted messages to their phone about what to expect before and after the operation.
“How did you keep such good track of me? I felt supported, watched, less alone,” the patient noted.
It was a small but important part of Houston Methodist’s never-ending digital transformation that rapidly accelerated as the pandemic unfolded. Leaders from the organization’s DIOP team — Digital Innovation Obsessed People — outlined during the AHA’s recent virtual Leadership Summit how they evaluate, prioritize and implement digital solutions throughout the system.
A Culture in Which Success Is Expected
DIOP is part of a larger innovation network at Houston Methodist that comprises 12 departments in the system that represent all areas of operations. The assumption is that solutions will go from pipeline to pilot with a strategy that assumes success until proven otherwise, says Roberta Schwartz, executive vice president and chief innovation officer.
Products are only graduated through the pipeline once they can demonstrate return on investment at the line level, unless the benefit is so great that it warrants system-level funding.
Last year, the innovation network helped scale the organization’s virtual care portfolio across its hospitals, ambulatory care and physician settings. The sprint led to:
- Scaling to 35,000-plus virtual visits between February and April — a 25,000% increase.
- Executing more than 300,000 ambulatory care virtual visits in 2020.
- Virtual urgent care visits soared to more than 30,000.
- The rollout of a virtual intensive care unit (VICU) program that covered all its hospitals and 360 ICU beds.
That lightspeed change would not have been possible without a digital-first culture, says Sarah Pletcher, M.D., vice president and executive medical director of virtual care, Houston Methodist. The VICU team responded to more than 3,500 alerts last year in which bedside teams pressed a button to receive instantaneous help.
3 Ways Houston Methodist Has Digitally Transformed
Digital Care Pathways
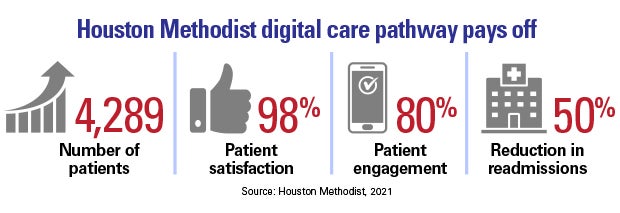
The innovation team set out to connect with patients in new ways, providing pre- and post-surgery educational support. The technology, often as simple as text messaging, generated 80% engagement levels and a 98% satisfaction rate among nearly 4,300 patients tracked. The initiative also led to a 50% reduction in readmissions. The system’s CareSense pathway sent more than 560,000 invitations for COVID-19 vaccinations, which led to more than 411,000 people getting their shots.
Voice Bots
The bots, deployed through the system’s phone lines, delivered COVID-19-related information to anxious patients when they needed it most without having to wait on hold, notes Josh Sol, administrative director of ambulatory innovation. The bots also were used to help staff update passwords and to help clinicians more quickly find the right information technology person to address their situations.
My Methodist Patient Tablets
These devices provided patients in isolation with access to streaming services like Netflix and Hulu and My Chart, which allows patients to collaborate with their care teams. The tablet also provides access to music therapy to calm patients as well as spiritual care and enables patients to talk with loved ones and use a translation service if needed. The tablets are automatically wiped clean of the prior user’s information to ensure security.
Other digital technologies the organization is exploring include smart speakers like Amazon’s Alexa with custom skills developed with the pharmacy to improve medication education and clinical voice technology to provide voice-powered and passive listening experiences for patients and clinicians, including voice commands that can be used in operating rooms.



