
4 Health Systems Transforming Care with AI
The use of AI in health care continues to grow. Recent data from an AHA Health IT supplemental survey show that the portion of hospitals utilizing predictive AI tools integrated with electronic health records increased from 66% in 2023 to 71% in 2024.
While the fastest growing use cases according to the Health IT survey data are those to support administrative efficiency, health systems are increasingly deploying AI to improve diagnosis, accelerate decision-making and support preventive care. Below are examples of how AHA members are applying AI in high-impact clinical settings.
(Note: This is not an exhaustive list of AHA members leveraging AI for detection and prevention.)
Detecting Congenital Heart Defects in Utero
 The prenatal diagnosis of congenital heart defects allows health care providers to ensure they have the right resources available (e.g., equipment and specialists) during delivery, preventing potentially detrimental treatment delays, board-certified obstetrician/gynecologist Nathan S. Fox, M.D., wrote in Med City News. However, detecting fetal heart abnormalities requires extensive training and is often difficult due to the small size of the heart and fetal movement. Many pregnant patients receive care in settings without access to maternal-fetal medicine specialists or pediatric cardiologists who can diagnose these issues.
The prenatal diagnosis of congenital heart defects allows health care providers to ensure they have the right resources available (e.g., equipment and specialists) during delivery, preventing potentially detrimental treatment delays, board-certified obstetrician/gynecologist Nathan S. Fox, M.D., wrote in Med City News. However, detecting fetal heart abnormalities requires extensive training and is often difficult due to the small size of the heart and fetal movement. Many pregnant patients receive care in settings without access to maternal-fetal medicine specialists or pediatric cardiologists who can diagnose these issues.
AI could change that by empowering community-based health care providers to diagnose fetal heart issues. For example, a study conducted by physicians at Mount Sinai West in New York City found that an AI tool designed to enhance ultrasound efficiency and accuracy increased detection of potential major congenital heart defects to more than 97%.
Identifying Peripartum Cardiomyopathy
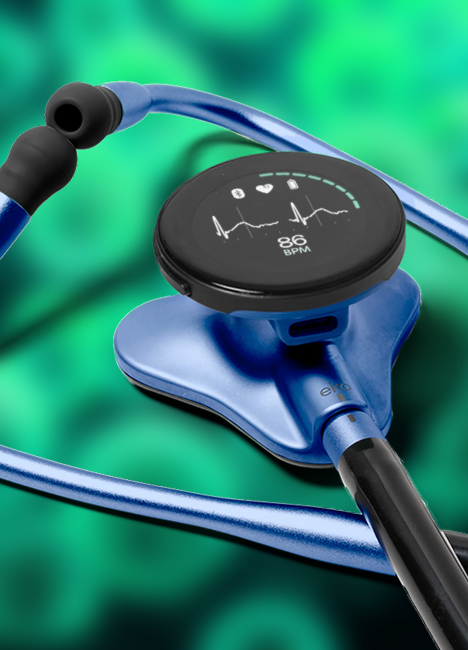 Researchers at the Mayo Clinic in Rochester, Minnesota, have found that an AI-powered digital stethoscope can help clinicians identify peripartum cardiomyopathy, a condition affecting approximately 1 in 2,000 pregnant people. The Mayo study showed that the AI-enabled stethoscope enabled physicians to diagnose twice as many patients with heart failure related to pregnancy, compared with traditional screening methods.
Researchers at the Mayo Clinic in Rochester, Minnesota, have found that an AI-powered digital stethoscope can help clinicians identify peripartum cardiomyopathy, a condition affecting approximately 1 in 2,000 pregnant people. The Mayo study showed that the AI-enabled stethoscope enabled physicians to diagnose twice as many patients with heart failure related to pregnancy, compared with traditional screening methods.
"This finding is significant. Cardiovascular disease, including cardiomyopathy, is the leading cause of maternal mortality in the U.S.," said Demilade A. Adedinsewo, M.D., a cardiologist at Mayo Clinic in Jacksonville, Florida, and the study’s lead investigator.
Accelerating Diagnosis and Decision-Making in Radiology
 Charlotte, North Carolina-based Advocate Health has integrated AI imaging models into clinical workflows to accelerate decision-making and improve patient outcomes.
Charlotte, North Carolina-based Advocate Health has integrated AI imaging models into clinical workflows to accelerate decision-making and improve patient outcomes.
“After rigorously testing and evaluating AI in radiology, we have come to the firm conclusion that responsibly deployed imaging AI tools, with oversight from expertly trained human providers, are a best practice in the specialty,” said Christopher Whitlow, M.D., enterprise chair of radiology at Wake Forest University School of Medicine, in a press release. “Whether you’re in a large city or a rural community, these technologies can help deliver diagnostic clarity and direction faster and more reliably than ever.”
An initial successful pilot study in October 2024 incorporated AI imaging models into Advocate’s diagnostic imaging process at 22 sites in Wisconsin and North Carolina, with the technology helping radiologists identify pulmonary embolisms, incidental pulmonary embolisms and intracranial hemorrhages. In July 2025, the health system announced plans to expand its use of AI in clinical imaging workflows to accelerate diagnosis and early intervention for a range of conditions, including rib fractures, cervical spine fractures, abdominal free air, pneumothorax, aortic dissection and brain aneurysms.
Advocate has projected that embedding Food and Drug Administration-approved AI models into imaging workflows will benefit almost 63,000 patients per year through earlier diagnoses and faster prioritization, according to internal modeling and early results from the pilot study.
Supporting Virtual Nursing and Preventing Falls
 Emory University Hospital Midtown in Atlanta launched a virtual nursing initiative in 2025, making it the first hospital within Atlanta-based Emory Healthcare to test new AI-powered technology and telehealth equipment for remote patient care and fall prevention. A team of nurses in a control room at another Emory hospital monitors and supports patients using a combination of AI, telehealth, hardware and software to complete tasks such as medication management and admissions paperwork.
Emory University Hospital Midtown in Atlanta launched a virtual nursing initiative in 2025, making it the first hospital within Atlanta-based Emory Healthcare to test new AI-powered technology and telehealth equipment for remote patient care and fall prevention. A team of nurses in a control room at another Emory hospital monitors and supports patients using a combination of AI, telehealth, hardware and software to complete tasks such as medication management and admissions paperwork.
Rooms on the medical/surgical floors of Emory University Hospital Midtown were outfitted with the AI and telehealth solutions. The virtual nursing setup includes Light Detection and Ranging (LIDAR) technology, which monitors patients in their rooms. If the system detects movement that could lead to a fall, an automated voice instructs the patient to stay in bed until the care team arrives to assist.
The Bottom Line: Responsibly Transforming Care Delivery with AI
The nonprofit health care research organization ECRI and the Institute for Safe Medication Practices (ISMP) recently noted in their annual patient safety concerns report that AI can improve diagnostic accuracy “by automating data retrieval, decreasing cognitive load, reducing cognitive biases and providing clinicians with information to help guide their decisions.” While taking steps to ensure responsible deployment is vital, AI can be a useful addition to clinicians’ toolbox.




