

How to Check the Pulse of Your Digital Behavioral Health Efforts

At the peak of New York state’s COVID-19 outbreak, Montefiore Medical Center in the Bronx was at the epicenter. As the pandemic stressed the organization’s resources, needs became particularly acute at Montefiore Behavioral Health Center, long noted for its open access care model in treating the area’s most impoverished patients.
“We were state of the art before the pandemic,” notes Thomas F. Betzler, M.D., executive clinical director. “Our rehospitalization rate was lower than the region and the state.”
But, with the overwhelming number of COVID-19 cases being treated at the Montefiore Medical Center, the organization had to rapidly change its operations. For the behavioral health center, that meant greatly expanding its already innovative use of digital solutions to connect with its patients. This would be needed to continue to serve the 250 to 300 behavioral health patients the center typically sees each day.
 Betzler explained in a recent AHA webinar how digital systems can enable an effective behavioral health strategy. Experience gained during a pre-pandemic pilot with the Valera Health app made for a smooth transition to expanding virtual care. The app connects patients with care teams to speed response time to hundreds of the center’s high-risk behavioral health patients during a critical time when face-to-face treatment was significantly hampered by COVID-19.
Betzler explained in a recent AHA webinar how digital systems can enable an effective behavioral health strategy. Experience gained during a pre-pandemic pilot with the Valera Health app made for a smooth transition to expanding virtual care. The app connects patients with care teams to speed response time to hundreds of the center’s high-risk behavioral health patients during a critical time when face-to-face treatment was significantly hampered by COVID-19.
Betzler says the app has been effective in working with high-risk patients, including those who are psychotic, have had multiple or recent suicide attempts or multiple recent hospitalizations. Indeed, in a pre-pandemic pilot with the app and more than 300 patients, nearly 72% remained in contact with their social worker weekly and talked with a psychiatrist at least once a month.
Likewise, the center’s reverse integrated care model employed before the pandemic, in which patients’ primary care needs were assessed at the time of their intake for behavior health issues, paid dividends. That gave providers instant access to more complete health data to assess patients — an important factor when virtual visits were soaring.
Now, with New York’s most severe surge behind it, Betzler is hoping the state will continue to reimburse for telepsychiatry and video visits and other efforts that have proven to increase access and better meet community needs. “This is the future,” he says.
Benchmarking Your Digital Health Efforts
Many health care organizations are on a similar path as Montefiore, even if their strategies and tactics may differ in deploying digital systems to optimize behavioral health access and efficiency. It’s part of an ongoing effort to improve workforce capacity, expand psychiatric and substance use-disorder treatment capabilities, and integrate physical and behavioral health.
To help with this effort, the AHA, in collaboration with the health care digital transformation consultancy AVIA, has created three free benchmarking resources for members — collectively called the AHA Digital Pulse. One of these tools, the Behavioral Health Pulse, helps organizations drive clinical innovation in behavioral health services and increase access and capacity.
A new AHA infographic provides a user map for the Digital Pulse and illustrates who might benefit from participating in each of the assessments in the platform.
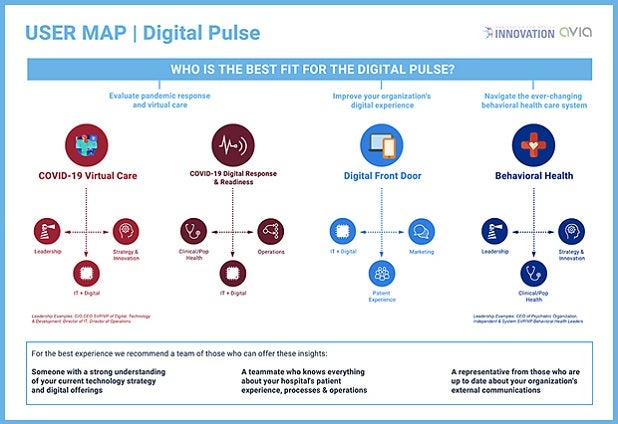
AHA’s Digital Pulse self-assessment tools can help organizations learn where existing capabilities can support scaling digital transformation, prioritize high-value solutions that can have the greatest impact and benchmark digital capabilities against those of peer organizations. In addition, the Pulse allows members to explore resources to help them accelerate progress and to see how they compare with peers who are also benchmarking progress with this resource.
Leslie Marsh, president and CEO, Lexington (Neb.) Regional Health Center, says the Digital Pulse has helped advance knowledge in her organization. “If we wanted to go a specific direction, [we’d ask] ‘Do we have the know-how and knowledge where we didn’t before?’ And now we do as a result of participating in the Digital Pulse.”
The Pulse is only one aspect of AVIA’s digital innovation platform — AVIA Connect — to which AHA members have full access with their AHA.org account. With Connect, members can assess their digital behavioral health capabilities and view a curated database of solution providers with which their peers have chosen to work; engage with peers in closed and open discussion groups; and view timely and relevant content on subjects of interest via the AHA online community.
The Behavioral Health Pulse is the third assessment release of the AHA Digital Pulse. As part of their membership, AHA hospitals and health systems also can take advantage of the Digital Front Door Pulse and COVID-19 Pulse. Liz Dean, executive director of strategy and business development of Riverwood Healthcare Center in Aitkin, Minn., says the Digital Front Door tool can be particularly helpful to organizations with tight resources.
The Behavioral Health Pulse comprises two main components: increasing access and capacity and driving clinical innovation. It addresses the following challenges:
Increasing Access and Capacity
- TeleMAT [medication-assisted treatment] services.
- Telemental services.
- Peer support services.
- On-demand behavioral health services.
Driving Clinical Innovation
- Behavioral health screening.
- Behavioral health integration.
- Emergency department-based mental health interventions.
- ED-based substance-use disorders.
By evaluating their organizations' capabilities in specific areas, members can see where they stand against their peers. The Behavioral Health Pulse will clearly and efficiently show what “good” looks like in the field and will point you toward those organizations that are performing well on specific measures.
Taking the Behavioral Health Pulse, the COVID-19 Pulse and the Digital Front Door Pulse will help you understand what capabilities are needed and give you access to valuable information and resources to inform your path forward.
“The Digital Front Door Pulse was really important for our organization. We’re a stand-alone community hospital,” says David Schreiner, president and CEO at Katherine Shaw Bethea Hospital. “The assessment was important for us to know not only where we are today, but to help us have a path going forward so that we could avoid those multiple distractions that are always out there.”
“We don’t have in-house experts and large teams to figure all this out, and we all wear so many hats, so we need partners to help us,” says Dean. “The COVID-19 Pulse helped us quickly identify virtual health solutions. We gained insights on best practices, resources and reassurance that we were on the right track. Because we used this tool, we were able to implement virtual solutions very quickly and efficiently.”



