

Futurescan 2026: 4 Insights That Will Shape Hospital Strategy

Hospitals and health systems must rethink traditional strategies and embrace bold transformation to remain financially strong amid policy, workforce and reimbursement challenges, according to the 2026 Futurescan report recently released by the Society for Health Care Strategy & Market Development (SHSMD), a professional membership group of the American Hospital Association (AHA).
As significant policy and reimbursement changes impact resources and access in the health care field, providers must carefully determine the best long-term strategy based on data analysis and not be afraid to revamp their culture, processes, technology, data integration and delivery capabilities.
Futurescan contains predictions from health care leaders surveyed about various topics related to the future of the field. Please see below for a sampling of key responses.
Produced in collaboration with the American College of Healthcare Executives since 1999, the report combines expert guidance with insights from thousands of hospital and health system executives to help leaders plan for the next five years.
Here Are Four Key Strategies from Futurescan 2026
1 | Take calculated risks — and don’t fear failure.
In today’s unpredictable world, hospitals and health systems must avoid employing a cautious “wait and see” strategy, John Poziemski, managing director and consulting innovation leader for Kaufman Hall, advises in the report.
“Don’t fear innovation,” Poziemski writes. “Many organizations are cautious about pursuing innovation. It’s not only OK to fail, to experiment in a meaningful way, but it’s necessary in the current market environment.”
For example, Kaufman Hall worked with a large health system that shut down and entirely rebuilt its urgent care enterprise, including dozens of sites, with a new organizational model after realizing the venture was failing to fulfill its intended purpose for the system.
2 | Partner with retailers to stay competitive.
“Retailers are increasingly following the money to develop sustainable models, and health systems that fail to collaborate with them risk losing out on significant opportunities,” says Chris Schrader, a partner on Oliver Wyman’s Health Services and Digital, Technology, and Analytics teams, according to the report.
For instance, in 2024, New Hyde Park, New York-based Northwell Health partnered with Instacart — which established a health division in 2022 — to increase access to healthy food for underserved populations. Pregnant patients who are food insecure can now receive nutrition guidance and support from Northwell and utilize Instacart Health Fresh Funds.
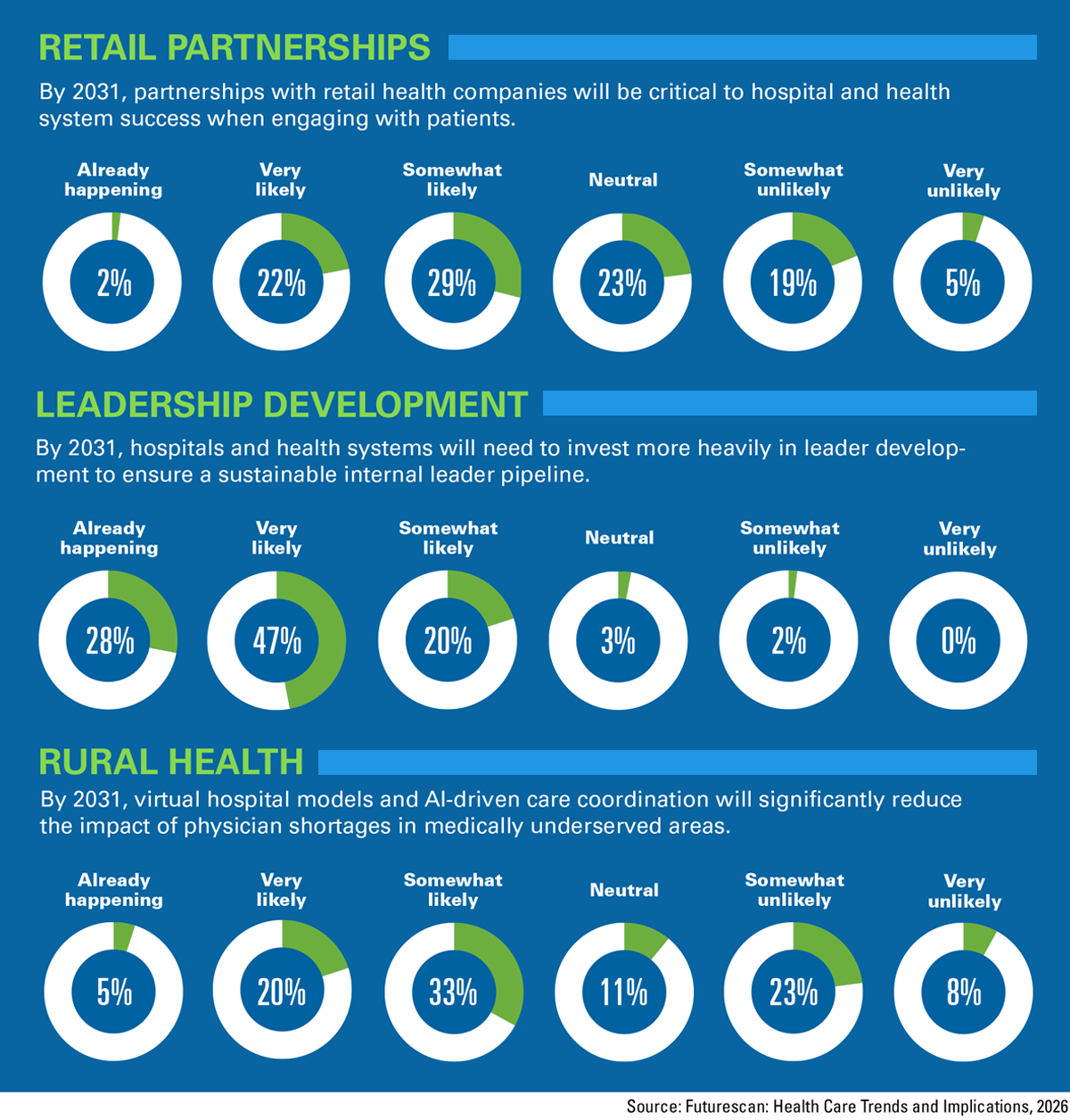
Approximately half (51%) of the health care executives surveyed for the 2026 Futurescan report agreed that partnerships with retail health organizations will be vital for hospital and health system success in engaging with patients by 2031.
3 | Invest in developing future leaders.
Nearly half (47%) of the health care executives surveyed for the report agreed that it’s very likely that hospitals and health systems will need to invest more heavily in leader development to support a sustainable internal pipeline by 2031.
When searching for future leaders within your organization, uncover latent potential by having conversations about aspirations and considering unconventional career trajectories as well as character, advises Olesea Azevedo, senior executive vice president and chief culture and transformation officer at Altamonte Springs, Florida-based AdventHealth.
Azevedo notes that leaders should have “the courage to grow, the curiosity to learn, and the heart to serve,” according to the report.
“By expanding our definition of who is ‘ready,’ we unlock possibilities in people who bring lived experience, passion and values-driven vision,” she says.
4 | Use technology to offset workforce shortages.
Approximately half (53%) of the health care executives who responded to the Futurescan 2026 survey agreed that AI-driven care and virtual hospital models are very or somewhat likely to significantly mitigate the effects of physician shortfalls in medically underserved communities by 2031.
In rural regions, technology that enables virtual care delivery is vital for hospitals and health systems grappling with workforce shortages and serving people living in remote areas that make accessing care a challenge. For example, in 2024, Sanford Health in Sioux Falls, South Dakota, opened a Virtual Care Center creating a direct connection to the health system’s rural hospitals and satellite clinics. Subsequently, patients in those areas no longer need to travel hundreds of miles for the care they need.
“It’s saving patients the costs associated with driving and fuel purchases and the need to take time away from work, to find reliable childcare, and to stay overnight for certain visits,” says Sanford Health President and CEO Bill Gassen, according to the report. “We’re able to meet people in their homes or in smaller storefront clinics that have nursing staff, basic imaging, and lab services available.”
The 2026 Futurescan report is free for SHSMD members and available for purchase for non-members. Explore the full report.
SHSMD is also hosting a webinar to review key findings from Futurescan 2026 on March 11 at noon CDT. The event is open to both SHSMD members and non-members. Learn more and register.




