Societal Factors That Influence Health
As cornerstones of their communities, hospitals and health systems play a role in addressing societal factors that influence the health of the patients and communities they serve. Focusing on societal factors benefits patient care and serves as an avenue to meet hospitals’ strategic goals including advancing equity, improving quality and outcomes, reducing costs, and building community engagement and trust.
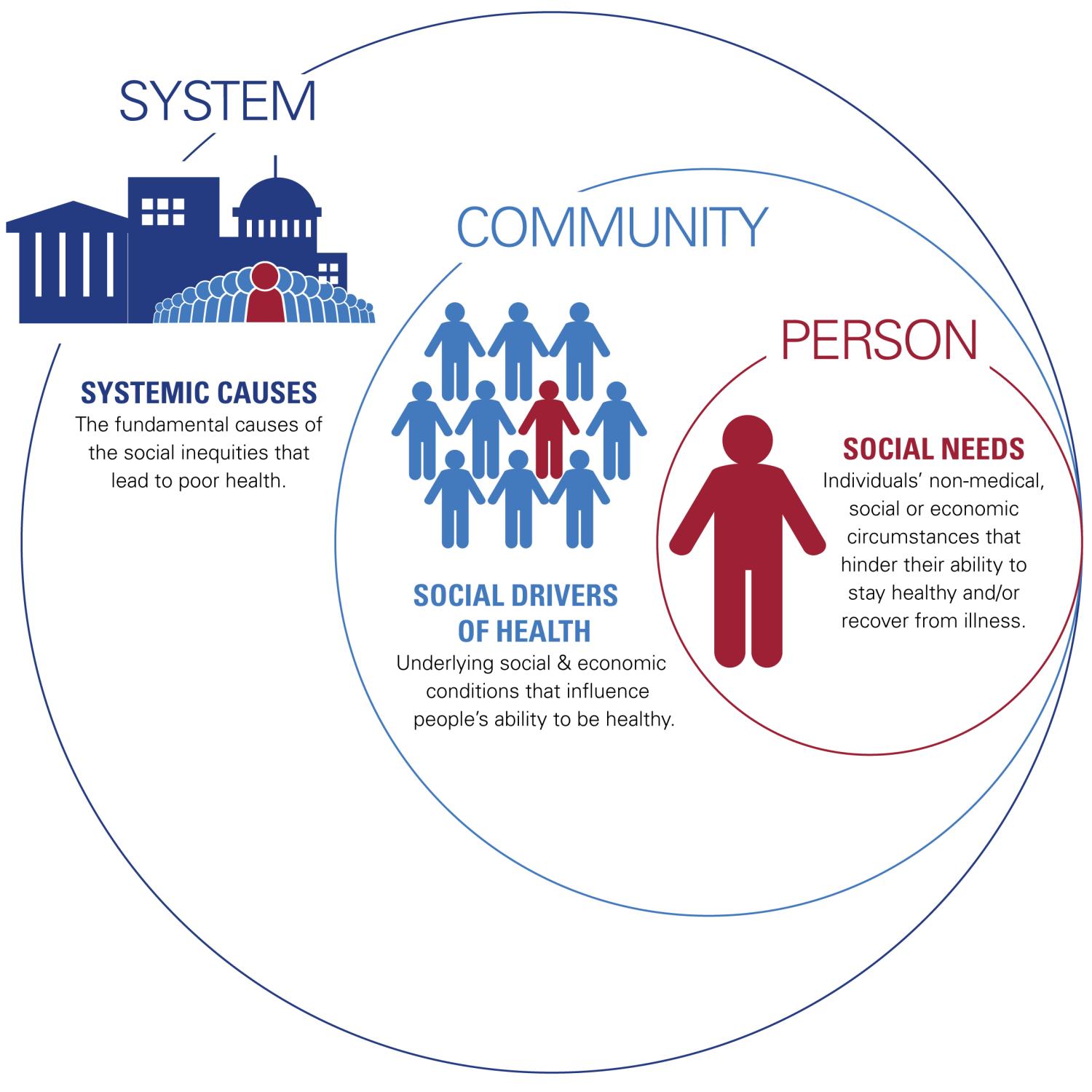
The AHA’s Societal Factors that Influence Health Framework is designed to guide hospitals’ strategies to identify patients' social needs, the social drivers of health in their communities and the systemic causes that lead to health inequities so all stakeholders can take action around these critical issues.
Societal Factors That Influence Health: A Framework for Hospitals
AHA Resources
Explore AHA’s growing repository of resources to support hospitals and their community stakeholders as they take action to address the societal factors that influence health.
Investing in the Power of Teams to Address Social Needs
Meeting patients’ social needs is a collaborative effort, which requires engagement of various professions from across the health care spectrum and community. Learn how Regional One Health and New-York Presbyterian Hospital improved health outcomes by leveraging specialized skills of care team members to identify and address the social needs of their patients.
Housing and Health
A Roadmap for the Future examines the impact of housing instability on individuals’ health and outlines opportunities and avenues for hospitals to reduce housing instability in their communities. This tool shares strategic considerations for how to tailor a housing strategy to meet community needs and case examples of how hospitals are addressing housing instability during COVID-19.
Screening for Social Needs: Guiding Care Teams to Engage Patients
Screening for Social Needs: Guiding Care Teams to Engage Patients is a tool to help hospitals and health systems facilitate sensitive conversations with patients about their nonmedical needs that may be a barrier to good health. It is the latest effort by The Value Initiative to promote the field’s work to drive value by lowering cost and improving outcomes.
ICD-10-CM Coding for Social Determinants of Health
Numerous studies have demonstrated a link between the social determinants of health and key health outcomes. AHA has worked to promote widespread use of ICD-10-CM codes that enable provider to collect data on the social determinants of health.
Using Z Codes to Improve Health Equity in Rural Indiana
Cameron Memorial Community Hospital, an independent critical access hospital in northeastern Indiana, shares how it embraced the use of ICD-10-CM Z codes to detect and address patients’ social needs as part of the hospital’s health equity strategy.
Value-based Payment to Support Health Equity
AHA’s The Value Initiative summarizes a conversation among two experts, Amol Navathe, M.D., assistant professor, medical ethics and health policy, University of Pennsylvania Perelman School of Medicine, and Mai Pham, M.D., president and CEO, Institute for Exceptional Care, about opportunities and challenges in implementing value-based payment models to improve health equity.
Addressing Social Determinants of Health Presentation
Social determinants of health – where we live, work and play – have tremendous affect on one’s health, and they can affect anyone, regardless of age, race, ethnicity. Help your organization and community better understand how social determinants impact your patients and neighbors as well as what hospitals are doing to address this important aspect of health, and what resources AHA has to help you further tackle related challenges including food insecurity and lack of transportation.
Social Determinants of Health Guides
AHA is producing a series of guides on how hospitals can address various social determinants of health. Below are the topics covered to date:
- Food Insecurity and the Role of Hospitals
- Housing and the Role of Hospitals
- Transportation and the Role of Hospitals
Social Determinants of Health Curriculum for Clinicians
To help clinicians address social determinants, the AHA’s Physician Alliance created a web-based virtual expedition to train and equip staff with how-to actions and companion resources. Modules include an overview of social determinants, introduction to upstream quality improvement, and a focus on addressing food and housing insecurity as well as transportation.
Strategies For Reimagining Health Care
AHA Transformation Talks
Learn more about Social Determinants: Leveraging the Community and Innovation to Improve Health and download the abstract or framework.









